Journal of Comprehensive Nursing Research and Care Volume 8 (2023), Article ID: JCNRC-188
https://doi.org/10.33790/jcnrc1100188Research Article
Preventing Nurse Burnout In New Graduates
Shan Gordon RN, BSN, DNPs, & Janice Thurmond DNP, APRN, Project Advisor
Department of Nursing, Murray State University, 1375 Chestnut St, Murray, KY 42071
Corresponding Author Details: Shan Gordon RN, BSN, DNPs, Department of Nursing, Murray State University, 1375 Chestnut St, Murray, KY 42071, United States.
Received date: 02nd May, 2023
Accepted date: 02nd June, 2023
Published date: 05th June, 2023
Citation: Gordon, S., & Thurmond, J., (2023). Preventing Nurse Burnout In New Graduates. J Comp Nurs Res Care 8(1):188.
Copyright: ©2023, This is an open-access article distributed under the terms of the Creative Commons Attribution License 4.0, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Abstract
Nurses comprise most of the healthcare workforce, and addressing burnout among newly graduated nurses could help alleviate it. This DNP project aimed to prevent nurse burnout among newly graduated nurses through an educational program about nurse burnout and methods to decrease it. A survey design was used to test the relationship between job stress and burnout in newly employed nurses. A presentation was given to newly hired nurses during their orientation period. It defined nurse burnout and discussed methods to decrease or prevent burnout. Nineteen recently graduated nurses were included. Participants were asked to complete the Perceived Stress Scale and Burnout Self-Test surveys after the presentation and at 30-, 60-, and 90-days using Survey Monkey. An ANOVA table was used to compare the results. New graduates perceived no stress before employment. Thirty days after hire, their ability to handle stress decreased, while the probability of their burnout rate increased. Sixty days after working, new graduates’ stress marginally increased while their ability to handle stress did not change, indicating their likelihood of burnout did not change. Therefore, their potential for burnout did not increase because their ability to handle stress did not change. Finally, after ninety days of employment, the graduate’s responses declined, making that data insignificant. Helping new graduate nurses develop coping skills to deal with transitioning to practice and learning pre-emptive strategies to lessen the effect of burnout will aid them in mitigating their symptoms of burnout and help maintain a vital workforce.
Keywords: Nursing, New graduates, Burnout, Resilience, Stress
Introduction
Nursing burnout is a common and expensive healthcare problem that affects nurses and patient care. According to the U.S. Bureau of Labor and Statistics, there will be an average of 194,000 openings for Registered Nurses annually [1]. Estimates of cost due to nurses leaving their positions due to burnout range from $11,000 to $90,000 per nurse, with up to $8.5 million associated with higher prices secondary to unfilled vacancies, training, and orientation [2]. Nurses comprise most of the healthcare workforce, and addressing burnout among newly graduated nurses could help alleviate it. For decades, burnout has had adverse effects on the healthcare system and has contributed to absenteeism, nurse turnover, and decreased patient satisfaction [3]. Educating these nurses on ways to connect with staff, be present and supportive, and ensure they find meaning and purpose in their role can improve retention and lessen the effects of burnout. Burnout in new graduate nurses begins in their undergraduate years. They experience burnout before entering the profession and are at a higher risk of leaving after 10-15 months [4]. Therefore, it is vital to provide guidance, support, and the appropriate resources to help newly graduated nurses thrive, be engaged, and be successful [5].
Results obtained from many studies revealed that newly graduated nurses needed a program to transition from the school setting into an actual working environment, and many needed to be equipped to deal with the demands of working in a healthcare setting. Newly graduated nurses experience a difference between their ideal and actual work conditions and must prepare for this discrepancy before graduation [6]. They feel inadequately prepared, so work overload and stress make them vulnerable to developing frustration and failure leading to burnout. Nursing is a demanding profession, and transitioning from student nurse to registered nurse can be challenging [7,8]. A period of shock leads to stress as they distinguish between what they learned as a student and experience as a new graduate [8].
The purpose of the study was to understand factors that influence student nurses' stress and provide strategies that can be designed to enhance their psychological adjustment to the workforce and prevent burnout. More importantly, it is necessary to solve the shortage of nurses by helping new graduate nurses adapt to the clinical setting as soon as they enter the profession [9-11].
Materials and Methods
Design
Approval for this study was obtained from Murray State University’s IRB board. This DNP project was a time–lagged quantitative empirical study of new graduate nurses employing survey analysis covering a timeline of 90 days. A survey design method was used to test the relationship between job stress and burnout in newly employed nurses. A presentation was given to newly employed nurses during their orientation period. The presentation defined nurse burnout and included discussion on methods to decrease or prevent burnout. Participants were asked to complete the Perceived Stress Scale and Burnout Self-Test surveys after the presentation, and at 30, 60, 90 days using Survey Monkey. It is a crucial project for nursing to prevent burnout and maintain an adequate nurse workforce. The adverse effects of job burnout have a detrimental impact on employees and hospital organizations and threaten patient care and safety [12].
Ethical Considerations
All surveys used for this project were stored on Survey Monkey. Survey Monkey is a username and password-protected website. Survey Monkey allowed participants to maintain anonymity from the DNP student. The DNP student only received notification that there was a reply to the surveys and a response to the questions, but there was no indication of who responded.
Background
A year before this study, the DNP student reviewed the literature to determine if any significance was found that new graduate nurses would benefit from such a project. After completing this review, it was determined that recent graduates benefited from programs before graduation on what to expect upon employment. The review also proved that the transition to practice programs after hire successfully maintained new graduates in the workforce.
Setting
This study occurred at a large magnet hospital, one of the most extensive healthcare systems and the fourth largest employer in the western region of Kentucky. This facility employs more than 34,000 individuals in their western area. They has received ANCC Magnet Recognition for providing nursing excellence the gold standard of nursing, and believe nurses are essential to providing quality and safety to patients and families. This organization is committed to offering nurses support and the necessary systems they need to provide safe, timely, efficient, effective, and patient-centered care (Mercy Health -Lourdes n.d.).
Sample
Participants in this project were new graduate nurses hired to begin their careers. A total of 19 new graduate nurses participated in this survey analysis. Unfortunately, two participants did not return a survey on days 30-90 after employment due to an inadequate email address. The sample size could undermine its validity [13].
Data Sources/Collection
Orientation schedules of newly hired nurses were obtained, and plans were made with the Professional Development staff of the organization to allow a thirty-minute Microsoft PowerPoint program during their orientation. This presentation included the origin of burnout, its definition, manifestations, prevalence, and outcomes. The program also included the challenges many new graduates face transitioning to practice. In addition, it offered insights into where burnout becomes a problem for young nurses. Finally, the presentation concluded with the skills needed to lessen or prevent nurse burnout. The program began with obtaining the signed consent of new graduate nurses present for the hospital orientation program. This consent was also to secure participation and provide the knowledge that all information provided by the graduates would be kept anonymous (see Appendix A). Secondly, a questionnaire called the Perceived Stress Scale was administered. This questionnaire aimed to determine the graduates' stress levels before transitioning to their new roles. Finally, the Microsoft PowerPoint program was presented. Post-surveys consisting of the Perceived Stress Scale and the Burnout Self-Test were sent to the participants using Survey Monkey by email 30, 60, and 90 days after the new graduates had been working, and they were given 30 days to complete each survey.
The Perceived Stress Scale consists of ten questions developed by Sheldon Cohen. It is a measure based on the psychological conceptualization of stress. The Perceived Stress Scale included ten questions which were rated on a five-point frequency of 1) Never, 2) Almost Never, 3) Sometimes, 4) Fairly Often, and 5) Very Often. Questions 1-3, 6, 9, and 10 are negatively worded, and questions 4, 5, 7, and 8 are positively framed (see Appendix B).
The Burnout Self-Test was developed by Mind Tools and consisted of 16 questions to identify burnout risks. This questionnaire was given at timed intervals after beginning employment, along with The Perceived Stress Scale. The Burnout Self-Test is a predictive measure of an individual's risk of developing burnout. The Burnout Self-Test included 16 questions and were also scored on a five-point scale of 1) Not At All, 2) Rarely, 3) Sometimes, 4) Often, and 5) Very Often. All questions are designed to address an individual’s level of burnout (see Appendix C).
Data Analysis/Statistical Methods
Data collection of the responses to these surveys was compiled through Survey Monkey. After that data was obtained, it was sent anonymously to a statistician to review and construct an ANOVA table to compare the results using Excel and MATLAB programs. The results were formulated for the time periods of 30, 60, and 90 days following the new graduate’s employment.
Results
The participants in this study were 19 new graduate nurses beginning their careers; unfortunately, two were lost in follow- up due to an inadequate email address. Data were compared using the ANOVA table, which produced data for each thirty-day timeline resulting in a P-value to express statistical significance. A P-value < 0.05 is considered statistically significant, and a P-value > 0.05 is not statistically significant and indicates that a relationship does not exist between variables [14].
Nineteen new graduates were given a pre-survey, the Perceived Stress scale, to evaluate how they rated their stress levels before beginning employment, establishing a baseline for further comparisons. After the initial survey, a PowerPoint presentation was given regarding pre-emptive ways to address stress and prevent burnout. Next, two surveys were given, the Perceived Stress Scale and the Burnout Self Test, to determine stress levels and burnout symptoms at 30, 60, and 90 days (see Appendix A, and B).
Perceived Stress Scale
In this survey, questions 1-3, 6, 9, and 10 are negatively worded, and questions 4, 5, 7, and 8 are positively framed.
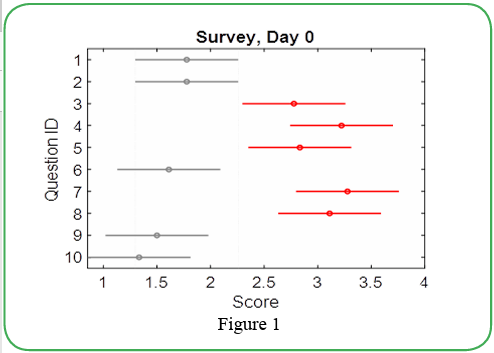
On Day 0, 19 new graduates showed that the average response to the negatively worded questions was less than the average response to the positively framed questions. Figure 1 demonstrates that answers to the negative questions are statistically different from positive ones, meaning there was minimal perceived stress before the students began employment. Responses to question 3 revealed an intermediate stress level. This might be associated with the everyday routine elevated stress levels (see Figure 1).
On day 30, only ten respondents had completed the surveys, and the average response for the negatively worded questions was less than that for the positively framed questions. Figure 2 answers for question 3 statistically overlap with most questions except questions 4 and 10. This indicates that the participant's ability to handle stress decreased (see Figure 2).
For day 60, the intermediate answer for the negatively worded questions was lower than the positively framed questions. Therefore, the average score for the negative questions was 1.8 for day 0 to 2.6 for day 60. In contrast, the average score for the positively worded questions did not change significantly, 3.1 for day 0 and 3.3 for day 60, which means that students perceived stress increased. At the same time, they felt confident in their ability to handle stress. On day 60, there is no statistical difference in responses for questions 1-10. This may have happened because the average answer for the negative questions and the average response for positive questions marginally increased (see Figure 3).
Ninety days after beginning employment, the number of respondents who answered the survey resulted in a small data set, and no conclusions could be drawn. The P-value from The Perceived Stress Scale on day 0 was 4.07162e-16, indicating a difference between the questions. However, the P-value on day 60 of the Perceived Stress Scale is P = 0.5173, meaning there are no significant differences in responses (see Appendix D).
Burnout Self-Test
This survey looks at how an individual feels about their job and experiences at work. It is an informal approach to assessing burnout.
On Day 30, the average response to question 16 was 3.7 and statistically different from the average response to questions 3, 4, 5, and 10, which is 1.9. Intermediate answers to the remaining questions range between 1.9 and 3.7. This indicates that the participants feel that their schedules or activities could be better planned due to their perceived lack of time. The average response to questions 1-16 is 2.4, indicating medium burnout due to stress during this period (see Figure 4).
On days 60 through 90, there are no statistical differences in the average response to questions 1-16. The overall average response for all questions was 2.6, which means that the burnout ratios among the participants did not increase because their ability to handle stress did not change. The P-values of the Burnout Self-Test on days 60 and 90, respectively, are P = 0.791 and P = 0.8123, meaning that there are no statistical differences in responses to the questions (see Appendix D).
Discussion
A PICOT question was developed to format and guide this project. The PICOT question is: In newly graduated nurses transitioning to practice, does education on nurse burnout enhance job retention and decrease burnout over three months? The project demonstrated that students beginning their employment were experiencing no stress. At three months, graduates experienced stress and the potential for burnout. At sixty days after hire, they rebounded with an ability to handle their stress and decrease their potential for burnout. However, the results were inclusive due to the low sample size and the number who responded to the surveys as the timeline progressed.
Interpretation
Data shows that students at the beginning of their employment identified minimal stress that could be attributed to everyday stressors. However, after thirty days of work, their ability to handle stress had decreased, and they were experiencing some associated burnout. Finally, at sixty days of being employed, their perceived stress levels increased while they felt confident in their ability to handle stress. It was during the thirty days after employment that 42% of new graduates reported they were more upset, more nervous, and stressed, could not cope with all that they had to do, were angered because of things that were outside of their control, and felt difficulties were piling up so high they could not overcome them. The results of the sixty-day improvement could support the association between a program to address stress and prevent burnout. Since there was a lower number of respondents, it can also be speculated that most graduates had left the institution or the profession.
Implications
The literature supports educating new graduates with the tools they need to enter the workforce to reduce stress and prevent burnout. Research demonstrates that the transition process for newly graduated nurses is stressful, and many new nurses leave the profession during this period. The current healthcare environment demands that new graduate nurses be ready to enter the workforce fully prepared. Unfortunately, many are unaware of their challenges, leading them to develop burnout and leave the profession (Shultz, n.d.). Therefore, it is vital to help nursing students transition from student to nurse and prepare for clinical practice [15]. Transitioning new graduates into a professional setting is complex, and reality shock is standard among newly graduated nurses entering the workforce. It is a phenomenon that nurse educators and healthcare administrators need to address. Ensuring work readiness in new graduates can decrease burnout and increase patient satisfaction [16].
Limitations
The most significant limitation of this project was the low sample size, and the participants came from only one healthcare organization. The number of students who responded to the surveys decreased as the timeline increased. This does not lend itself to any firm conclusions. Self-report questionnaires can be subject to response bias due to situational influences. Specialty areas where nurses work may also influence perceived stress and burnout, which was not addressed in this study [12]. Gathering data on age and gender could have been of benefit to determine if these factors influenced stress and the potential for burnout. Studies that examine ways to prevent burnout are numerous. Exploring profiles of nurses who present the most significant risk for burnout and those capable of handling it and not burnout could be beneficial to develop coping strategies, personal resources, and communication skills that prevent burnout.
Recommendations
Burnout continues to be a significant problem in nursing nationwide. Solutions must come from healthcare organizations and governmental legislation. As new graduate nurses work to improve their self-care and direct their professional development, they will face challenges to their well-being [17]. Helping these new graduate nurses develop coping skills to deal with the shock of transitioning to practice and learning pre-emptive strategies to lessen the effect of burnout will aid them in alleviating their symptoms of burnout and help maintain a vital workforce [18]. Presently, all nurses struggle to cope with emotional exhaustion, depersonalization, and a decreased sense of personal accomplishment.
Individual coping strategies may offer immediate support to new nurses. They are cost-effective and simple interventions that can reduce or prevent the effects of nurse burnout. Studies that examine ways to avoid burnout are numerous. Exploring profiles of nurses who present the most significant risk for burnout and those capable of handling it and not burnout could be beneficial to develop coping strategies, personal resources, and communication skills to prevent it. Burnout continues to be a growing problem in the nursing community, and more research, techniques, and interventions to mitigate or inhibit its effects are essential. Both educational and practical interventions are needed to facilitate improvement in job retention. "A candle's fire cannot continue burning if insufficient resources exist [19]".
Competing interest:
The authors declare that they have no competing interests.
Acknowledgements
Words cannot express my gratitude to my professor and clinical advisor, Dr. Janice Thurmond, for her invaluable patience and guidance. She provided unwavering support, keeping me focused on the journey ahead. I am also deeply indebted to Dr. Sergiy Markutsya for the knowledge and expertise he shared with me in performing the statistical analysis of this project. He created the figures and tables, provided a factual review, and helped edit the manuscript. With his words, I could determine the statistics' results. Moreover, he made them understandable and straightforward. Finally, Dr. Gary Harper shared his knowledge and expertise in presenting my program to his hospital employees.
I thank Marc Glass for editing and proofreading many papers and giving advice and suggestions during this undertaking. In addition, his moral support throughout this whole process has been invaluable.
Lastly, I'd like to mention my family; my mother, Creo Christian, endured having to read many manuscripts and give her feedback. Unfortunately, my father, Robert Christian, passed shy from this final project, but his faith in me will continue. My son, Ian Wilson, was one of my greatest cheerleaders who never stopped encouraging me to continue. Finally, I would be remiss in not mentioning my husband, Max Gordon, whose love and faith in me kept my spirits and motivation high during this process. I could not have made this journey without him and my Lord and Savior, Jesus Christ.
References
Bureau of Labor Statistics, U.S. Department of Labor, Occupational Outlook Handbook, Registered Nurses, at https:// www.bls.gov/ooh/healthcare/registered-nurses.htm(visited February 14, 2023).View
Kelly, L. A., Gee, P. M., & Butler, R. J. (2021). Impact of nurse burnout on organizational and position turnover. Nursing Outlook, 69(1), 96–102. https://doi.org/10.1016/j. outlook.2020.06.008View
Cañadas-De la Fuente, G. A., Vargas, C., San Luis, C., García, I., Cañadas, G. R., & De la Fuente, E. I. (2015). Risk factors and prevalence of burnout syndrome in the nursing profession. International Journal of Nursing Studies, 52(1), 240–249. https://doi.org/10.1016/j.ijnurstu.2014.07.001View
Dames, S. (2019a). The interplay of developmental factors that impact congruence and the ability to thrive among new graduate nurses: A qualitative study of the interplay as students transition to professional practice. Nurse Education in Practice, 36, 47 53. https://doi.org/10.1016/j.nepr.2019.02.013View
Jones, C. (2008). Revisiting nurse turnover costs. JONA: The Journal of Nursing Administration, 38(1), 11–18. https://doi. org/10.1097/01.nna.0000295636.03216.6fView
Yu, M., & Lee, H. (2018). Impact of resilience and job involvement on turnover intention of new graduate nurses using structural equation modeling. Japan Journal of Nursing Science, 15(4), 351–362. https://doi.org/10.1111/jjns.12210View
Gardiner, I., & Sheen, J. (2016). Graduate nurse experiences of support: A review. Nurse Education Today, 40, 7–12. https://doi. org/10.1016/j.nedt.2016.01.016View
Irwin, K. M., Saathoff, A., Janz, D. A., & Long, C. (2020). Resiliency program for new graduate nurses. Journal for Nurses in Professional Development, 37(1), 35–39. https://doi. org/10.1097/nnd.0000000000000678View
Xie, J., Li, J., Wang, S., Li, L., Wang, K., Duan, Y., Liu, Q., Zhong, Z., Ding, S., & Cheng, A. K. (2020). Job burnout and its influencing factors among newly graduated nurses: A cross sectional study. Journal of Clinical Nursing, 30(3-4), 508–517. https://doi.org/10.1111/jocn.15567View
McKenzie, R., Miller, S., Cope, V., & Brand, G. (2021). Transition experiences of newly qualified registered graduate nurses employed in a neonatal intensive care unit. Intensive and Critical Care Nursing, 67, 103112. https://doi.org/10.1016/j. iccn.2021.103112View
Frögéli, E., Rudman, A., Ljótsson, B., & Gustavsson, P. (2020). Preventing stress-related ill health among new registered nurses by supporting engagement in proactive behaviors—a randomized controlled trial. Worldviews on Evidence-Based Nursing, 17(3), 202–212. https://doi.org/10.1111/wvn.12442View
Boamah, S. A., Read, E. A., & Spence Laschinger, H. K. (2016). Factors influencing new graduate nurse burnout development, job satisfaction and patient care quality: A time-lagged study. Journal of Advanced Nursing, 73(5), 1182–1195. https://doi. org/10.1111/jan.13215View
Faber & Fonseca, (2014).How sample size influences research outcomes.Dental Press J Orthod;19(4):27-9. doi: 10.1590/2176 9451.19.4.027-029.ebo.View
Capili, B., & Anastasi, J. K. (2023). Improving the validity of causal inferences in observational studies. AJN, American Journal of Nursing, 123(1), 45–49. https://doi.org/10.1097/01. naj.0000911536.51764.47View
Rees, C. S., Heritage, B., Osseiran-Moisson, R., Chamberlain, D., Cusack, L., Anderson, J., Terry, V., Rogers, C., Hemsworth, D., Cross, W., & Hegney, D. G. (2016). Can we predict burnout among student nurses? an exploration of the icwr-1 model of individual psychological resilience. Frontiers in Psychology, 7. https://doi.org/10.3389/fpsyg.2016.01072View
Labrague, L. J., & Santos, J. A. (2020). Transition shock and newly graduated nurses' job outcomes and select patient outcomes: A cross-sectional study. Journal of Nursing Management, 28(5), 1070–1079. https://doi.org/10.1111/ jonm.13033View
Couser, G., Chesak, S., & Cutshall, S. (2020c). Developing a course to promote self-care for nurses to address burnout. OJIN: The Online Journal of Issues in Nursing, 25(3). https://doi. org/10.3912/ojin.vol25no03ppt55View
Lee, J. S., & Akhtar, S. (2011). Effects of the workplace social context and job content on nurse burnout. Human Resource Management, 50(2), 227–245. https://doi.org/10.1002/hrm.20421View
Basar, U., & Basim, N. (2016). A cross-sectional survey on consequences of nurses' burnout: Moderating role of organizational politics. Journal of Advanced Nursing, 72(8), 1838–1850. https://doi.org/10.1111/jan.12958View