Journal of Public Health Issues and Practices Volume 3 (2019), Article ID: JPHIP-149
https://doi.org/10.33790/jphip1100149Review Article
Smart Homes for Health: Promises and Concerns for Aging Societies
Sun Goo Lee
1Underwood International College, Yonsei University, Veritas B, Rm 436, 85 Songdogwahak-ro, Yeonsugu, Incheon, South Korea.
Corresponding Author Details: Sun Goo Lee, Department of Science, Technology and Policy, Yonsei University, Veritas B, Rm 436, 85 Songdogwahakro, Yeonsugu, Incheon, South Korea. E-mail: sungoolee@yonsei.ac.kr
Received date: 20th August, 2019
Accepted date: 30th October, 2019
Published date: 31st October, 2019
Citation: Lee, S.G. (2019). Smart Homes for Health: Promises and Concerns for Aging Societies. J Pub Health Issue Pract 3: 149.
Copyright: ©2019, This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Abstract
Objectives: In aging or aged societies, smart homes for health provide an option for older people to age with dignity and independence, while imposing minimal additional responsibilities on others. The goal of this paper is to review two major concerns related to smart homes to which policymakers should pay attention.
Methods: This paper reviews extant research on the current state of related new technologies and analyzes potential problems based on literature on data privacy and equity.
Results: First, smart homes face privacy violation risks because they provide sensitive personal information to various entities. Second, because smart homes are relatively costly to build and maintain, they are more likely to be available to a limited segment of the population.
Discussion: Since many countries are currently introducing smart homes, proper policies need to be devised in order to prevent these negative consequences.
Key words: Aging, Smart Homes for Health, Policy, Data privacy, Equity
Introduction
The world is aging rapidly. Approximately 12.3% of the global population is aged 60 and older, and this figure is expected to increase to almost 22% by 2050 [1]. This trend is even more remarkable in high-income countries (HICs) and upper-middle-income countries (UMICs). Nearly half (48.9%) of the populations of HICs and UMICs are projected to be older than 60 by 2030, compared to the global average of 16.5% [2]. By 2050, 16.6% of the populations of these countries will be aged over 80, compared to the world average of 4.5% [2].
Such a fast pace of aging presents several challenges for HICs and UMICs [3]. First, society faces an increase in its responsibilities toward the older population [4]. Studies of population health have shown that age almost always stands out as the single most powerful predictor of a person’s state of health [2]. Physician visits and medications are costly, and specialized facilities such as nursing homes are also expensive [4]. Consequently, an increase in the number of older people is generally correlated with an increase in healthcare spending. In the United States (US), for example, people aged over 65 spent an average of $1,215 on healthcare in 2011, while people of all ages spent an average of $703 [5].
In addition to the increased spending, an increase in the number of older people is likely to place heavy responsibilities on their caregivers, including family members and friends. Older people require assistance in their daily lives, whether they are in their homes or facilities. Caregivers in aging (or aged) societies often express emotional difficulties and physical limitations in fulfilling their duties [6]. Therefore, an important goal in an aging (or aged) society is to control healthcare expenditures and caregivers’ loads.
Another challenge these societies are encountering is establishing an environment where older people can age without compromising their dignity. Usually, worsened health conditions result in increased dependence and limited social connectivity, which tend to leave older people frustrated and dejected. Dependency, isolation, and helplessness contradict the concept of “aging well” declared by the United Nations namely, aging with independence, participation, dignity, care, and self-fulfillment [7]. These societies should therefore seek ways to improve the dependency and isolation of their older populations.
When these two primary goals are considered, smart homes seem to be an attractive residence option in HICs and UMICs. Smart homes that promote the health of older people (hereafter,“smart homes for health”) empower older people to manage their health conditions with the help of technologies and lead independent and socially connected lives in their communities [4,8]. As a result of extended independence, older people spend less time in and money on healthcare facilities and require less help from caregivers [4].
While many governments of HICs and UMICs are actively trying this new form of residence, policy discussion has been very limited to homes’ effectiveness, mainly concerning technological efficacy and older people’s acceptance of new technologies [4]. Few studies have touched upon the ethical concerns related to smart homes for older people, the scope of discussion being limited to the effects of different sensor designs on older people’s perceived protection of privacy [4,9]. As discussed later in this paper, smart homes for health have great potential to have negative side effects, and a lack of policy safeguards could leave societies vulnerable to the misuse of the technologies.
In this context, this paper reviews the positive contributions smart homes can make to health in aging (or aged) societies. This paper then suggests two concerns that policymakers should carefully consider in setting policies for smart homes. First, this paper reviews data privacy issues. Data privacy requires policymakers’ attention because smart homes for older people’s health are premised on collecting and using residents’ sensitive data. Second, this paper addresses equity concerns. Both financial and geographical inequities are likely to arise because smart homes use expensive up-to-date technologies. This study concludes that the successful application of smart home technologies for older people requires policymakers to address these concerns at the stage of adoption.
Potential Value of Smart Homes for Health
Among their many strengths, the outstanding attribute of smart homes for health is their ability to provide assistance to older residents so they may continue to lead active, functionally capable, independent lives within their communities [8,10]. When smart homes for health were not available, older people with compromised health conditions had no other option than to relocate to special facilities where their health and security would be better protected [11]. Such a change in the living environment is, however, reported to cause feelings of isolation and attendant mental and physical deterioration [12-14]. The Madrid International Plan of Action on Ageing and its Political Declaration (here after, the Madrid Plan) highlights the importance of “aging in place” in this regard [15].
Systematic reviews of the effects of smart home technologies that enable “aging in place” show that both preventive and therapeutic services tend to have positive effects in the domains of physical health, social participation, environmental aspects, and psychological health [16]. Preventive services, such as fall detection and the monitoring of chronic heart diseases, reduce fears and feelings of insecurity and enhance autonomy by generating data that enable timely interventions and provide residents adequate support [16]. Some of the main contributors to depression and difficulty with medication schedules include loneliness, boredom, isolation, and limited social interaction [16]. Here, information and communication technology (ICT) can be used to provide personalized support for time orientation, sensory awareness, communication, and recreational activities. These prior studies have concluded that these technologies enable older people to continue their lives with dignity through extended independence, social participation, and self-fulfillment [7,16].
In addition, because this type of residence eliminates health risks for older residents and empowers them to manage their health conditions by modifying their health behaviors, it is likely to reduce healthcare spending and caregivers’ responsibilities. Most illnesses from which older people suffer are chronic, such as hypertension, hyperlipidemia, diabetes, and arthritis [17]. For such illnesses, the management of health in daily life is usually effective enough to reduce the number of physician visits and dependence on medication, which translates into a substantial reduction of healthcare costs. Smart homes for health also substitute or supplement caregivers’ roles; examples of this include the monitoring of medication uptake and reminders of medical appointments. In research studies, caregivers have expressed that smart homes for health are effective in alleviating their burdens [18].
Many HICs and UMICs witnessing surges in their older populations have been striving to implement this form of residence in their countries. As a result, smart homes are readily available in many HICs and UMICs where developed technology is already in use and trained specialists can maintain the technology system effectively. For example, under the European Union’s Active Assisted Living (AAL) Programme, 24 countries including Canada, France, and the United Kingdom have initiated projects to implement AAL in policy [19].
As members of the International Electrotechnical Commission’s (IEC) Systems Committee on Assisted Living (SyC AAL), 25 countries including China, Japan, the Republic of Korea, and the US have been working to develop interoperational AAL technologies [20]. The IEC’s database shows that there are nearly 500 use cases of AAL services that deal with a wide variety of older people’s needs [21]. Now that many HICs and UMICs have already conducted pilot studies at multiple sites [6,22-26], it is only a matter of time before this type of residence becomes available in those countries.
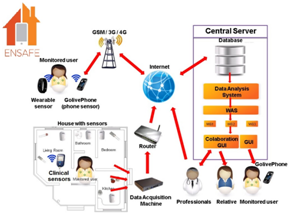
Figure: 1 Example of the mechanism of smart homes for health. (Source: ENSAFE, Active and Assisted Living Programme)
Policy Concerns
Although smart home technologies have been developing rapidly enough to make them a near-future option in many countries, efforts have predominantly focused on users’ acceptance and the efficiency of the new technologies. Regarding ethics and policy, only a couple of studies have briefly mentioned that there may be some privacy concerns, and the topic has not been exploredfurther [27,28]. This section examines two major concerns that policymakers should be mindful of whendesigning policies for smart homes for health.
Data Privacy
To receive accurate and effective services in smart homes, the resident needs to provide a wide range of information necessary to determine which service will help the resident control risk factors and remain healthy and active. For this purpose, the smart home system is critically premised upon accurate and up-to-date information.
The dementia management program is a good illustration of how smart homes for health can help older people continue to lead active lives in their communities. Let us say that 80-year old Jane, the resident and end user of the service, lives in Residence A and has registered for a dementia-related service. The system will activate sensors to monitor her lifestyle, as well as behavioral patterns associated with dementia. For example, if Jane were to leave home in the middle of night, supposing that she had never done so, her caretakers and security company would be notified, and wearable sensors would trace where she was. As physical exercise helps to slow the progress of dementia, Jane will receive messages reminding her to take a walk if she remains overly sedentary. If Jane is using the toilet too often, signaling that she is eating much more frequently than before, she would be booked for a checkup on the progress of her dementia and to confirm that she is taking her medication as required. Based on the results of the checkup, the system would take subsequent actions to monitor her health and provide the necessary coaching and assistance.
Such a personalized service requires several kinds of information. The first type of information is the residence information—namely, where the resident in need of service, identifiable under the name A, is living. Second, the system needs information regarding the general health risks of the resident; this includes age, sex, body temperature, height, weight, ethnicity, education level, income level, and so on. Third, the system requires information about the resident’s health condition, including their blood pressure and body mass index (BMI) and data regarding any medical diagnoses, as well as the medical history of both the resident and their family members. Finally, the system needs lifestyle and behavioral information related to the health condition of the resident. Examples of lifestyle and behavioral information include: how much the resident exercises on a daily basis, their degree of social interaction with others, what the resident eats on a daily basis, and whether the resident is compliant with medication instruction. By analyzing such information comprehensively, the smart home system can identify each resident’s health problems, monitor behavior that could either improve or worsen health conditions, provide immediate assistance when the resident is in need of help, and dispense services that could modify health behaviors, thereby addressing risk factors.
However, the use of the aforementioned information for healthcare services entails a substantial risk of privacy violation for several reasons. First, this bundle of information is basically used in a personally identifiable way. If information is de-identified to protect privacy (i.e., making it impossible to identify the subject of the information), it cannot be used to provide personalized services for that particular resident. While some de-identification measures such as pseudonymization prevent the system from being hacked during the transmission of information, once the information reaches an information user, it needs to be restored in an identifiable form; for example, the security company needs an identifiable form of information to take appropriate action in a given situation.
Second, the information collected and used by a smart home system is highly sensitive in nature. Health information collected by such a system reveals nearly everything about the resident’s health and daily life. One of the most recent examples of smart home technology is a pressure-sensing toilet seat that measures the patient’s blood pressure and health through his or her bowel movements [29]. Other similar sensors collect behavioral and lifestyle information, including what, when, and how someone eats. They also record when someone typically goes to bed and wakes up, and what bedtime activities they enjoy (including sexual activity). The more accurate smart home services aim to be, the more information their systems need to monitor and analyze.
Consequently, if the information is handed over to anyone other than those involved in providing the services, as Warren et al. [30] note, “what is whispered in the closet shall be proclaimed from the house-tops.” Residents’ private lives can be undermined and their right to privacy seriously violated [31]. Such violations are deemed more serious because the privacy at stake concerns things that happen in the home a place where an individual is expected to have the utmost level of freedom and non-interference [31].
Third, some information collected in smart homes, such as sexual orientation or weight, can evoke social discrimination in a community. Such information can also result in employment or insurance discrimination [32]. Some pieces of health information and family history regarding certain illnesses reveal not only the status of the resident’s health but also that of his or her family members. Many illnesses tend to run in the family; therefore, a father having hypertension, diabetes, or dementia signals that his child has an increased risk of such illness. As a result, social, employment, and insurance discrimination may be extended to family members.
Fourth, there is an increased risk of privacy violation in smart home settings because their services require that numerous entities share information about residents. It is not practically feasible that a single entity, be it a government or a private company, collect and process the requisite information, provide a wide range of services, and receive feedback from the residents. The types of services range from providing lifestyle coaching to dispatching a security agent or medical professional in liaison with hospitals. Therefore, in order for different entities specializing in providing certain services to coordinate effectively, they need to share sensitive information about the residents. Keeping track of information flow becomes difficult when information starts to circulate among different entities especially when fast circulation is required to maintain the system accuracy and effectiveness of the smart homes. Naturally, there is an increased risk of information being used without the permission of the residents, or of the residents losing track of the information flow.
As such, the risk of privacy violation is substantial in smart homes, which use integrated bundles of highly sensitive, personally identifiable information about every resident in need of service— although the technology that has enabled the collecting and processing of such integrated data is what makes customized healthcare services possible. Therefore, it is important that policies are set up to maximize the benefits of this new technology while minimizing the potential for privacy violations, as the attendant results will be catastrophic and irreversible.
Equity Concerns
Smart homes can be accessible to a certain segment of the population a demographic of increasing significance in an aging (or aged) society. However, the fact that different groups may have different degrees of access to smart homes for health may raise equity concerns. Inequity, as defined by theWorld Health Organization in Whitehead’s widely cited report, refers to differences in health that are not only unnecessary and avoidable but also unfair and unjust [33]. A widely used definition of injustice involves the degree of choice. For example, where people have little or no choice in their living and working conditions, the resulting health differences are more likely to be considered unjust than those resulting from health risks experienced voluntarily [33]. The sense of injustice increases for groups where disadvantages cluster together and reinforce one another, making such groups particularly vulnerable to low levels of health [33]. In this sense, smart homes could entail problems of economic and geographical inequity. First, with regard to economic inequity, smart homes with new ICTs and high-tech sensors are likely to be more costly than other traditional forms of residences. While prices for new technologies may eventually decrease in the long run, homes with these technologies will definitely be more expensive than those without them. In addition, the ICT systems of smart homes require regular maintenance, incurring additional expenses for residents. Moreover, the process of obtaining consent for information processing, as well as keeping track of information, also requires time and effort, which also translates into further expenses. Consequently, smart homes can be an option limited to older people who can afford high-priced residences.
Geographical inequity is also probable because smart homes are more likely to be available in urban areas. As observed in pilot studies, securing personnel resources for the maintenance of hightech homes poses a challenge to the success of scaling up smart home use [27]. It is likely that residences using new technologies will be more feasible in urban areas where there is a workforce to operate and maintain the system, as seen in the case of smart cities [34,35]. In addition, on average, people in urban areas tend to be more affluent than those in rural areas, which means that there should be a greater demand in urban environments.
That people in rural areas may have less access to smart homes is ironic, considering that it is rural areas that are most in need of such facilities. This is because rural areas usually have a significantly smaller number of clinics and hospitals, resulting in limited access to healthcare. In addition, older people in rural areas tend to be lesseducated resulting in the twofold problem of having less access to healthcare and less exposure to the information necessary to prevent or mitigate illness [36].
Since smart homes can be a significant social determinant of older people’s health, unequal access to them can exacerbate inequities in health [37,38]. Different levels of access to care in healthcare institutions have already been proven to produce dramatic changes in health [39], and smart homes can bring about even more dramatic results because they affect health behaviors around the clock.
Conclusion
As implied by the results of pilot studies at many different sites in a number of countries, careful planning will determine how successfully this new type of residence will improve residents’ quality of life [27]. From society’s perspective, smart homes for health can be beneficial only when policies are established to prevent the misuse of this new form of residence. Policymakers should carefully review the possible dangers associated with this new residence and design policies to prevent them [27]. Currently, a barrier to the successful adoption of smart homes relates to “the absence of ethical frameworks to underpin them” [24].
For policymakers to set safeguards against the potential downsides of smart homes for health, active research in the field is essential. Research efforts are required to accurately assess the pros and cons of smart homes for health and to suggest how policies should regulate smart homes for health, so that social benefits are maximized while harm is kept to a minimum.
Conflicts of interest/Competing interests
Authors report no conflict or competing interest.
References
United Nations Populations Fund. (n.d.) (2018) Ageing.View
United Nations. (2015) World population ageing 2015. (Online), June 26, 2018.View
Peek, S.T.M., Aarts, S., & Wouters, E.J.M. (2017). Can smart home technology deliver on the promise of independent living? A critical reflection based on the perspectives of older adults. In J. van Hoof, G. Demiris, & E. Wouters (Eds.), Handbook of smart homes, health care and well-being 203–214.View
Schulz, R., Wahl, H-W., Matthews, J. T., DeVito Dabbs, A., Beach, S.R., Czaja S.J. (2014). Advancing the aging and technology agenda in gerontology. The Gerontologist 55: 724–734.View
Fried, T.R., Bradley, E.H., Williams, C.S., & Tinetti, M.E. (2001). Functional disability and health care expenditures for older persons. Archives of Internal Medicine 161: 2602–2607.View
Aquilano, M., Cavallo, F., Bonaccorsi, E.M.R., Rovini, E., & Filippi, M...(2012). Ambient assisted living and ageing: Preliminary results of RITA project. In Engineering in medicine and biology society (EMBC), 2012 Annual International Conference of the Institute of Electrical and Electronics Engineers (IEEE) 5823– 5826.View
WHO. (n.d.). Global age-friendly cities project.View
Morris, M.E., Adair, B., Ozanne, E., Kurowski, W., & Miller, K... (2014). Smart technologies to enhance social connectedness in older people who live at home. Aus J Ageing 33: 142–152.View
Lorenzen-Huber, L., Boutain, M.L., Camp, L.J., Shankar, K., & Connelly, K.H...(2011) Privacy, technology, and aging: A proposed framework. Ageing Int 36: 232–252.View
Skubic, M., Alexander, G., Popescu, M., Rantz, M., Keller, J... (2009). A smart home application to eldercare: Current status and lessons learned. Technology and Health Care 17: 183–201.View
O’Leary, P. (1991). Toward healthy aging: Human needs and nursing response. J Gerontological Nurs 17: 45.
Johnson, R.A. (1999). Helping older adults adjust to relocation: Nursing interventions and issues. In L. Swanson & T. Tripp- Riemer (Eds.), Transitions in the older adult 52–72).
Manion, P.S., & Rantz, M.J. (1995). Relocation stress syndrome: A comprehensive plan for long-term care admissions: The relocation stress syndrome diagnosis helps nurses identify patients at risk. Geriatric Nurs 16: 108–112.View
Rantz, M., & Egan, K. Reducing death from translocation syndrome. American Journal of Nursing, 87(9), 1351–1353.
United Nations (2002). Political declaration and Madrid international plan of action on ageing.View
Siegel, C., Dorner, T.E. (2017). Information technologies for active and assisted living: Influences to the quality of life of an ageing society. Int J Med Informatics 100: 32–45.View
Prince, M.J., Wu, F., Guo, Y., Gutierrez Robledo, L.M., O’Donnell M...(2015). The burden of disease in older people and implications for health policy and practice. The Lancet 385: 549–562.View
Rialle, V., Ollivet, C., Guigui, C., & Hervé, C. (2008). What do family caregivers of Alzheimer’s disease patients desire in smart home technologies? Methods of Information in Med 47: 63–69.View
Active and Assisted Living Programme (n.d.). Our projects.View
IEC (n.d.) SyC AAL Membership.View
Eichelberg, M., Rolker-Denker, L., & Helmer, A. (2014) AAL use cases and integration profiles. AAL Joint Programme.
Barbabella, F., Chiatti, C., Masera, F., Bonfranceschi, F., Rimland, J.M. (2014). Experimentation of an integrated system of services and AAL solutions for Alzheimer’s disease patients and their caregivers in Marche: The UP-TECH project. In S. Longhi, P. Siciliano, M. Germani, & A. Monteriù (Eds.), Ambient assisted living 157–165.View
Biocca, L., Casacci, P., D’Innocenzo, A., Di Pasquale, D., & Fabbri, F...(2014). Smart technologies in social housing: Methodology and first results of the HOST project experimentation activities.” In S. Longhi, P. Siciliano, M. Germani, & A. Monteriù (Eds.), Ambient assisted living 303–312.
Fisk, M,J. (2003). Social alarms to telecare: Older people’s services in transition. Bristol: Policy Press.View
Moschetti, A., Fiorini, L., Aquilano, M., Cavallo, F., Dario, P... (2013). Ambient assisted living: Italian Forum 2013. Preliminary Findings of the AALIANCE2 Ambient Assisted Living Roadmap: 335–342.View
Moschetti, A., Fiorini, L., Aquilano, M., Cavallo, F., Dario, P... (2014). Preliminary findings of the AALIANCE2 ambient assisted living roadmap. In S. Longhi, P. Siciliano, M. Germani, & A. Monteriù (Eds.), Ambient assisted living 335–342.
Hayn, D., & Schreier, G. (2017). Assistive solutions in practice: Experiences from AAL pilot regions in Austria. In Health informatics meets ehealth: Digital insight–information-driven health &care. Proceedings of the 11th EHealth 2017 Conference 236: 184.View
Reeder, B., Chung, J., Lazar, A., Joe, J., & Demiris, G...(2013). Testing a theory-based mobility monitoring protocol using inhome sensors: A feasibility study. Res Gerontological Nurs 6: 253–263.View
Liberatore, S. (2016). Smart toilets that analyze your poop and ultrasonic baths that 3D scan your internal organs: Google patent reveals plan for bathroom that can monitor your health.View
Warren, S.D., & Brandeis, L.D. (1890). The right to privacy. Harvard Law Rev 4: 193–220.
Solove, D.J., & Schwartz, P. (2014). Information privacy law. Amsterdam: Wolters Kluwer.
Chemerinsky, E. (2016). Constitutional law: Principles and policies. Alphen aan den Rijn, Netherlands: Wolters Kluwer.
Whitehead, M. (1991). The concepts and principles of equity and health. Health Promotion Int 6: 217–228.View
Nam, T., & Pardo, T.A. (2011). Conceptualizing smart city with dimensions of technology, people, and institutions. In Proceedings of the 12thAnnual International Digital Government Research Conference: Digital Government Innovation in Challenging Times 282–291.View
Neirotti, P., De Marco, A., Cagliano, A.C., Mangano, G., Scorrano, F...(2014). Current trends in smart city initiatives: Some stylised facts. Cities 38: 25–36.View
Hale, T.M., Cotten, S.R., Drentea, P., & Goldner, M. (2010) Rural-urban differences in general and health-related internet use. Am Behav Sci 53: 1304–1325.View
Casey, M.M., Call, K.T., & Klingner, J.M. (2001). Are rural residents less likely to obtain recommended preventive healthcare services? Am J Prevent Med 21: 182–188.View
WHO (2008). Closing the gap in a generation: Health equity through action on the social determinants of health.View
Demiris, G., Rantz, M.J., Aud, M.A., Marek, K.D., & Tyrer, H.W... (2004). Older adults’ attitudes towards and perceptions of “smart home” technologies: A pilot study. Med Informatics and the Internet Med 29: 87–94.View

