Journal of Public Health Issues and Practices Volume 5 (2021), Article ID: JPHIP-183
https://doi.org/10.33790/jphip1100183Research Article
Examining the Intersection of Alcohol Use and Hookups among Transgender College Students: A Descriptive Study
Alice Ma, PhD, MPH1*, Brittany D. Chambers, PhD, MPH2, Amanda E. Tanner, PhD, MPH3, Kari C. Kugler, PhD, MPH4, Jeffrey J. Milroy, DrPH, MPH3 , and David L. Wyrick, PhD3
1Department of Applied Health, Southern Illinois University Edwardsville, Edwardsville, IL, United States.
2Preterm Birth Initiative, Department of Epidemiology and Biostatistics, The University of California, San Francisco, San Francisco, CA, United States.
3Department of Public Health Education, The University of North Carolina at Greensboro, Greensboro, NC, United States.
4Department of Biobehavioral Health, The Pennsylvania State University, University Park, PA, United States.
Corresponding Author Details: Alice Ma, PhD, MPH, CHES, Department of Applied Health, Southern Illinois University, Edwardsville, Campus Box 1126, Edwardsville, IL 62026-1126, United States. E-mail: ama@siue.edu
Received date: 13th July, 2021
Accepted date: 25th August, 2021
Published date: 27th August, 2021
Citation:Ma, A., Chambers, B. D., Tanner, A. E., Kugler, K. C., Milroy, J. J., & Wyrick, D. L. (2021). Examining the Inter-section of Alcohol Use and Hookups among Transgender College Students: A Descriptive Study. J Pub Health Issue Pract 5(2): 183.
Copyright:©2021, This is an open-access article distributed under the terms of the Creative Commons Attribution License 4.0, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Abstract
We examined the intersection of alcohol use and hookups among transgender college students to identify sexual behaviors that may reduce negative hookup experiences. Our analytic sample included US college students who identified as transgender (n=36; 11 trans men and 25 trans women). Descriptive analyses were performed using the Online College Social Life Survey (2005–2011) to describe transgender students’ alcohol use, hookups, and related sexual behaviors. Twenty-five (69.4%) transgender students reported a hookup since entering college. The majority (n=19; 76.0%) of hookups included only non-penetrative sexual behaviors. Of these hookups, nearly half (n=9; 47.4%) reported heavy drinking. Some condom use was reported with penetrative hookups. This suggests that transgender students use some lower risk strategies during hookups. Alcohol use was high, which has implications for the consistent use of these behaviors to reduce negative hookup experiences.
Key Words: Transgender, College Students, Alcohol Use, Hookups, Sexual Behaviors
Introduction
Youth and young adults (i.e., ages 15 to 24) account for approximately half of all new sexually transmitted infections (STIs) [1], and transgender persons (i.e., persons whose gender identity or expression differ from their sex assigned at birth) are more than three times more likely to report a new HIV diagnosis than the national average [2]. Despite these data, research on transgender young adults is limited, including for transgender college students who may face additional challenges as they navigate the transition and adjustment to college. They may experience adult identity development characteristic of emerging adulthood, which may be further complicated by the lack of transgender-specific programming during their academic tenure [3]. These challenges may impact their engagement in health-promotive behaviors, including sexual health behaviors that reduce STI acquisition (e.g., condom use) [4]. Given that college can increase opportunities for young adults to engage in health risk behaviors, examining the intersection of alcohol use and sexual behaviors, including hookups (i.e., casual sexual encounters), can illuminate priorities in messaging to support transgender students’ sexual health.
Although alcohol use and sexual encounters are a normative part of the college experience, these behaviors may exacerbate health risks for transgender students and lead to negative consequences (e.g., STI acquisition and negative hookup experiences). Alcohol use during hookups may prevent or disrupt the engagement in some preventive behaviors (e.g., condom use) [5]. Alcohol use prevalence, including for heavy episodic (i.e., binge) drinking, is nearly as high among transgender college students as cisgender students (i.e., persons whose gender identity or expression align with their sex assigned at birth) [6,7]. However, transgender students who have engaged in heavy episodic drinking do so more frequently than their cisgender counterparts, which may increase the likelihood of negative consequences (e.g., drinking during hookups and inconsistent condom use) [8]. Given that transgender students may be a subpopulation of college students whose health needs are not being met [9,10], examining the intersection of alcohol use and hookups may highlight gaps in messaging to reduce negative hookup experiences and support transgender student health [11,12].
The present analysis is a direct response to the Institute of Medicine’s [13] call to expand research on transgender persons’ health. The purpose of this descriptive study was to examine the intersection of alcohol use and hookups among transgender college students to identify sexual behaviors that may reduce negative hookup experiences to inform the development and framing of risk reduction and sexual health promotion messaging.
Materials and Methods
Participants and Procedures
The Online College Social Life Survey (OCSLS; 2005–2011) was used to examine transgender students’ experiences. The OCSLS includes data from a convenience sample of college students (N=24,131) from 22 colleges and universities across the United States (US) who completed a self-administered survey about their sociodemographic characteristics and behaviors; detailed information about the methods is discussed elsewhere [14]. The analytic sample included 36 students who identified as transgender (male-to-female [trans women] or female-to-male [trans men]; <0.1% of the total sample) and represented 14 colleges and universities. The Institutional Review Board at the University of North Carolina at Greensboro approved the study protocol.
Measures
Alcohol use during or prior to a hookup was assessed as an open-ended question for various types of drinks (i.e., beers, glasses of wine, mixed drinks or shots, and malt beverages). Respondents entered the number of drinks for each type with the prompt: “How much alcohol did you drink before or during the hook up?” We measured alcohol use by dichotomizing students’ responses to denote lower and higher risk drinking behaviors across all types of drinks: any alcohol or heavy episodic drinking. Any alcohol use was defined as (1) respondents who did not drink to (2) those who drank at least one alcoholic drink during or prior to a hookup. To measure heavy episodic drinking, given that the effects of heavy drinking may differ by gender and the lack of standardization on measuring alcohol use with transgender persons, we used standard cut-offs for respondents’ heavy episodic drinking (four or more drinks on one occasion for females, and five or more for males) calculated based on both their assigned sex (i.e., sex assigned at birth) and their transgender identity (i.e., trans women or trans men).
Students’ most recent hookup since entering college and the sexual behaviors that occurred were assessed with the prompt: “Use whatever definition of hookup you and your friends generally use. It doesn’t have to include sex to count if you and your friends would call it a hookup.” We extended previous operationalizations of sexual behaviors that compared different types of sexual activities (e.g., vaginal sex, oral sex, and genital stimulation) by grouping and dichotomizing most recent hookup into those that included (1) lower risk and (2) higher risk sexual behaviors to examine activities associated with generally less or more STI risk that could result in less or more negative hookup experiences, respectively [15]. Lower risk hookup behaviors included touching, genital stimulation, kissing, and/or oral sex. We included oral sex in this category because it is typically associated with lower STI risk compared to vaginal and anal sex [16]. Higher risk hookup behaviors included having vaginal and/or anal sex exclusively or in conjunction with touching, genital stimulation, kissing, and/or oral sex.
Related sexual behaviors included lower risk sexual activities (i.e., touching, genital stimulation, kissing, and/or oral sex) and condom use (yes/no) during respondents’ most recent hookup.
Analyses
Descriptive statistics were performed using IBM SPSS version 23 (Armonk, NY). We assessed the prevalence and intersection of respondents’ alcohol use, most recent hookup, and related sexual behaviors using crosstabs.
Results
The majority of transgender college students identified as trans women (n=25; 69.4%), White (n=22; 61.1%), and heterosexual (n=17; 47.2%). Over half (n=25, 69.4%) reported having a hookup since entering college. Slightly over half (n=13, 52.0%) reported using alcohol prior to or during the hookup. The majority of these hookups included heavy episodic drinking measured by assigned sex (n=11; 84.6%) and transgender identity (n=10; 77%) (see Table 1).
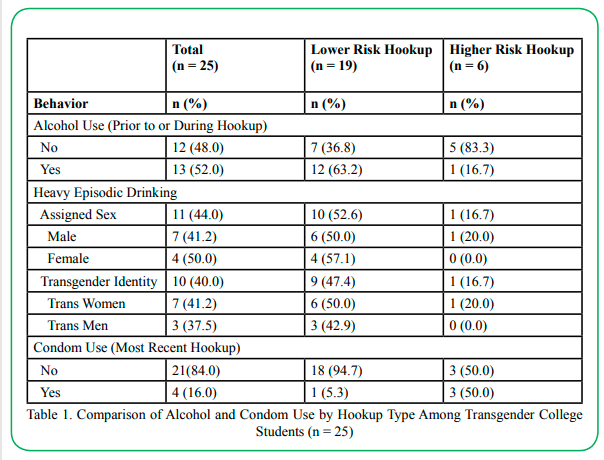
Table 1.Comparison of Alcohol and Condom Use by Hookup Type Among Transgender College Students (n = 25)
Among the 25 transgender students who reported a hookup, over three-fourths (n=19; 76.0%) reported participating in lower risk sexual behaviors. Over half (n=12; 63.2%) who had lower risk hookups reported using alcohol prior to or during the hookup. Heavy episodic drinking was reported in about half of the lower risk hookups (n=9, 47.4% measured by transgender identity; n=10; 52.6% measured by assigned sex). Approximately one-fourth (n=6; 24.0%) of students who had a hookup reported higher risk sexual behaviors. Half (n=3) who had a higher risk hookup reported using a condom.
Discussion
Our study addresses a subpopulation who is often absent from the existing literature on college students’ health behaviors, yet remain understudied and underserved in the literature and in practice. Despite our limited sample, we identified notable findings that warrant further study. Our results suggest that transgender students’ most recent hookups may include some lower risk sexual behaviors, such as condom use and kissing, that pose a lower risk for STI acquisition. Although other reasons may explain this finding (e.g., in a public location where penetrative sex is difficult), these lower risk sexual behaviors could be a result of feelings of disconnect between students’ physical appearance and their (trans)gender identity, particularly if these students have not (and desire to) medically and surgically transition [17]. They may not desire certain intimate interactions during hookups (e.g., penetrative sex). Although definitive data of the percentage of transgender students who engage in hookups are unknown, speculative, or combined with sexual minority students (e.g., gay and lesbian), research suggests that their hookups may be challenging the dominant culture pervasive on college campuses by emphasizing communication and exploring other pleasurable sexual behaviors [18]. Future research should examine hookup behaviors in the context of positive sexuality (e.g., pleasure and intimacy).
Alcohol use tended to be high among transgender students in this study, which is similar to prior work [6,7]. Research suggests that transgender students report more heavy episodic drinking events than cisgender students, despite cisgender males’ greater prevalence of heavy episodic drinking [8]. These drinking behaviors have implications for the consistent use of lower risk strategies during hookups and the risk for STI acquisition among transgender students.
Several limitations should be considered when interpreting our findings. The results from our small sample are unlikely to represent all transgender students (e.g., nonbinary identities). Further, the lack of an operational definition of ‘hookup’ in the original dataset may have resulted in the underreporting of hookup behaviors. More research is needed to understand the relationship between hookups and alcohol use and the factors motivating this relationship. It is also unclear how alcohol is metabolized differently for trans women and trans men and the implications for measuring heavy episodic drinking. Larger studies of transgender students are essential to more fully illuminate their experiences to inform the development and framing of risk reduction and sexual health promotion messaging on college campuses in the US.
Competing Interests:
The authors declare that they have no competing interests.
References
Centers for Disease Control and Prevention (CDC). (2017). Sexually transmitted diseases. Retrieved from https://www.cdc. gov/std/life-stages-populations/adolescents-youngadults.htmView
Centers for Disease Control and Prevention (CDC). (2019). HIV among transgender people. Retrieved from https://www. cdc.gov/hiv/group/gender/transgender/index.html. View
Schmidt, C. K., Miles, J. R., & Welsh, A. C. (2011). Perceived discrimination and social support: The influences on career development and college adjustment of LGBT college students. Journal of Career Development, 38(4), 293–309.View
Lewis, M. A., Rees, M., Logan, D. E., Kaysen, D. L., & Kilmer, J. R. (2010). Use of drinking protective behavioral strategies in association to sex-related alcohol negative consequences. Psychology of Addictive Behaviors, 24(2), 229–238.View
LaBrie, J. W., Hummer, J. F., Ghaidarov, T. M., Lac, A., & Kenney, S. R. (2014). Hooking up in the college context: The event-level effects of alcohol use and partner familiarity on hookup behaviors and contentment. Journal of Sex Research, 51(1), 62–73.View
Hotton, A. L., Garofalo, R., Kuhns, L. M., & Johnson, A. K. (2013). Substance use as a mediator of the relationship between life stress and sexual risk among young transgender women. AIDS Education and Prevention, 25(1), 62–71.View
Reisner, S. L., Gamarel, K. E., Dunham, E., Hopwood, R., & Hwahng, S. (2013). Female-to-male transmasculine adult health: A mixed-methods community-based needs assessment. Journal of the American Psychiatric Nurses Association, 19(5), 293–303.View
Coulter, R. W., Blosnich, J. R., Bukowski, L. A., Herrick, A. L., Siconolfi, D. E., & Stall, R. D. (2015). Differences in alcohol use and alcohol-related problems between transgender-and nontransgender-identified young adults. Drug and Alcohol Dependence, 154, 251–259.View
Grossman, A. H., & D'augelli, A. R. (2006). Transgender youth: Invisible and vulnerable. Journal of Homosexuality, 51(1), 111– 128.View
Wilson, E. C., Garofalo, R., Harris, D. R., & Belzer, M. (2010). Sexual risk taking among transgender male-to-female youths with different partner types. American Journal of Public Health, 100(8), 1500–1505.View
Centers for Disease Control and Prevention (CDC). (2020a). Sexual risk behaviors. Retrieved from https://www.cdc.gov/ healthyyouth/sexualbehaviors/index.htmView
Singh, A. A., Hays, D. G., & Watson, L. S. (2011). Resilience strategies of transgender individuals. Journal of Counseling & Development, 89(1), 20–27. View
Institute of Medicine. (2011). The health of lesbian, gay, bisexual, and transgender people. Washington, DC: The National Academies Press.View
Armstrong, E. A., England, P., & Fogarty, A. C. (2012). Accounting for women’s orgasm and sexual enjoyment in college hookups and relationships. American Sociological Review, 77(3), 435–462.View
Kuperberg, A., & Padgett, J. E. (2015). Meeting contexts, sex, and variation by gender, partner's gender, and class standing. Journal of Sex Research, 52(5), 517–531. View
Centers for Disease Control and Prevention (CDC). (2020b). STD risk and oral sex. Retrieved from https://www.cdc.gov/std/ healthcomm/stdfact-stdriskandoralsex.htmView
McGuire, J. K., Doty, J. L., Catalpa, J. M., & Ola, C. (2016). Body image in transgender young people. Body Image, 18, 96–107.View
Lamont, E., Roach, T., & Kahn, S. (2018). Navigating campus hookup culture: LGBTQ students and college hookups. Sociological Forum, 33(4), 1000–1022.View

