Journal of Public Health Issues and Practices Volume 6 (2022), Article ID: JPHIP-195
https://doi.org/10.33790/jphip1100195Research Article
Analysis of Student Perceptions Before and After Interprofessional International Medical Mission APPEs to Honduras
Craig Kimble, PharmD, MBA, MS, BCACP, TTS*, Tyler Clay, PharmD, BCPS, Robert Stanton, PharmD, MBA, BCPS, Amber Payne, BA, CPHT, and Omar Attarabeen, R.Ph., PhD
School of Pharmacy, Marshall University, Huntington, WV, USA.
Corresponding Author Details: Craig Kimble, PharmD, MBA, MS, BCACP, TTS, Associate Professor of Pharmacy Practice, Administration, and Research, Director of Experiential Learning/ Manager of Clinical Support Services, Marshall University School of Pharmacy, United States. E-mail: craig.kimble@marshall.edu
Received date: 02nd February, 2022
Accepted date: 18th February, 2022
Published date: 21st February, 2022
Citation: Kimble, C., Clay, T., Stanton, R., Payne, A., & Attarabeen, O., (2022). Analysis of Student Perceptionsbefore and After Interprofessional International Medical Mission APPEs to Honduras. J Pub Health Issue Pract 6(1): 195.
Copyright: ©2022, This is an open-access article distributed under the terms of the Creative Commons Attribution License 4.0, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Abstract
Objectives: This study evaluated student perceptions before and after completing a five-week Advanced Pharmacy Practice Experience (APPE) in International Healthcare focused on Medical Missions. Our objective was to understand how a medical mission APPE course meets student expectations, expanded interprofessional skills, and the impact the medical mission APPEs had on student’s cultural sensitivity and empathetic approach to patient care.
Methods: Two anonymous surveys were used to assess APPE student’s perceptions. These were conducted over 2 years with the first survey administered prior to trip departure. The second survey was administered after the in-country experience but prior to the end of the course. Survey results were compared to identify changes in perspectives related to providing patient care and to ensure students met course objectives. Additionally, in the surveys, students were asked to reflect on learning experiences including interprofessional clinics, medication distribution, empathy, and the Honduran healthcare system.
Results: Student’s primary motivation for taking this APPE elective was their desire to help others. Students reflected on the difficulties in communication with patients who spoke another language where access to technology was limited and they had to rely on interpreters. Prior to trip, a large percentage of the students on the survey did not demonstrate an understanding of the depth of poverty experienced in Honduras. Post–trip perceptions confirmed the change in perception versus reality when experiencing life in a developing country. Survey results suggested this APPE experience was a life changing one for them (67%) and changed their perception of patients as a healthcare provider (83%).
Conclusions: Results of this study demonstrate the value of exposing students to healthcare in a developing country as a component of the APPE curriculum. Even more important is recognizing the need for schools of pharmacy, experiential consortiums, and professional organizations to partner to ensure the continuation of these experiences post-pandemic. Students indicated this was a life-changing experience, recommended this as a course for other students to take, and stated this course would markedly affect them in their approach to providing empathetic patient care.
Key Words: International, Interprofessional, APPE, Empathy, Medical Mission
Background and Purpose
International Medical Mission Advanced Pharmacy Practice Experiences (APPEs) are experiential learning courses that give pharmacy students an opportunity to engage in the study and practice of health-care delivery abroad. The courses are completed in a foreign country which is medically and economically disadvantaged and are designed to give the student experiences in providing culturally competent interdisciplinary patient care. Literature has been previously published on medical mission trips through schools of pharmacy and medicine, addressing an overall description of the experience as an innovative teaching opportunity [1-5]. Our study however utilized pre- and post- surveys to compare student expectations prior to the APPE course and reflections post-course to evaluate students approach and appreciation for cultural similarities and differences in health care. Additionally, our APPE course design focuses on the medical efforts or planning and delivering a medical clinic versus any spiritual aspects. These courses present an excellent learning platform for students as related to infectious disease, poverty, empathy, travel medicine, interdisciplinary care, and chronic disease as documented in previous literature [1-7]. Development of the student’s skills in these key subject areas is an important component to providing compassionate care as a healthcare provider.
Educational Activity and Setting
The course in our program is a structured as a 5-week APPE elective with goals and objectives focused on planning and providing an International Medical Mission. Students learning experiences includetrip planning, supply procurement, and providing free health care to rural patients in Honduras, with an emphasis on pre-trip perceptions and post trip reflections. Students build upon previous didactic learning and introductory pharmacy practice experiences (IPPEs) to apply knowledge in a clinic medical mission operation. Many practice experiences are interdisciplinary in nature. Trips are coordinated with our university’s school of medicine (general practice, surgery, OB/GYN, and other specialties), nurse practitioners, nurses, and dentistry, with pharmacy students completing experiences in each area. Unlike other international APPEs, Students spend less time learning the health care system operations, regulatory environment, and payment systems in another country and more time in providing personal health care services to patients in need of direct care. To achieve the course’s foundational objectives, students worked with preceptors to develop clinical responsibility, provide inter professional care, understand population health disease state management, and develop an understanding about poverty and the culture of Honduras [2,4,7]. In addition, students have the opportunity to develop their skills and ability to provide care to those experiencing social determinants of health (SDOH). SDOH and their resultant impact are observed directly by students and include poverty, lack of potable water, limited transportation infrastructure, poor sanitation and malnutrition. These SDOH predispose patients in these clinics to chronic disease such as diabetes, heart disease, and obesity. Through this structured approach, students learn to develop an empathetic approach to care and why it is important to continue help them become more compassionate educators and caregivers.
The Office of Experiential Learning delivered an overview presentation of the course to interested students as part of the APPE education efforts prior to the course selection and match process. An informational session was conducted with interested students prior to the trip to discuss cost, travel requirements, enrollment, and other logistics. Students were given a period of time to decide if they wanted to pursue the experience considering these factors. APPE students who decided to enroll in the course met with faculty to discuss the syllabi and learning objectives for the course. In addition, students and faculty completed pre-trip education and planning. All attendees received basic background information and information related to potential risks which might be encountered (e.g. malaria, cholera, passport requirements, etc.). Students were given timelines to complete pre-trip requirements.
Students began the course weeks prior to the actual medical mission trip. Early in the course, students meet with faculty to discuss the culture of Honduras, living conditions, and challenges they will encounter while in Honduras. A learning goal with pre-trip education is to build cultural sensitivity and awareness along with communication skills and knowledge about diseases and challenges they will encounter. The course also incorporates the process of preparation and coordination of logistics for the trip and interdisciplinary collaboration. Students coordinate efforts with a faculty member, which include constructing a formulary for use in the patient care clinics which is similar to those in other medical mission trips [8]. Students were responsible for aiding in collection of medical supplies for the clinic and pre-packing medication for transport. They also had the task of aiding in fundraising efforts to run the clinics, purchase medications, and help pay for medical devices which could be left behind to improve care for future clinics.
The in-country medical mission clinic portion of the APPE is usually around a week in duration. Students work in multiple locations or clinic sites. Pharmacy students traveled with a pharmacist preceptor, nurses, physicians, nurse practitioner students, medical students, interpreters, and security. Groups ranged in size from as few as 12 up to as many as 47 personnel. These trips were planned in coordination with the medical students at the Marshall University Joan C. Edwards School of Medicine or in conjunction with Global Medical Brigades. Most clinic sites are very rural in nature. Students provided care for between 328 – 2800 patients per week and worked between 12-14 hours per day, plus a commute time approximately two hours each way. The most common disease states encountered by the students included chronic obstructive pulmonary disease (COPD), ischemic heart disease, diabetes, acute pain, and acute respiratory infections. The group saw patients in three to five different communities per week varying by the year travelled.
In-country experiences were purposefully developed to maximize the impact on the student’s empathy as a caregiver and to develop their inter professional skills. Students’ primary preceptors were school of pharmacy faculty but students also rotated through different stations including patient intake, triage, medical clinic, dentistry, ophthalmology, pharmacy, and patient counseling. In these stations, students worked with other health care professionals from various disciplines who were not the direct preceptor completing assigned tasks. Stations included time with physicians, medical students, nurse practitioners, nurses, pharmacists, or staff from the Global Medical Brigades. During the trip, students completed a structured end of the day debrief and reflection on the day’s activities, received general education about healthcare in Honduras, and shared reflection on their own unique perceptions.
Upon return from Honduras, students were required to complete a guided reflection paper with questions which helped students reflect and detail their experience. There were prompting questions related to cultural sensitivity, empathy, treatment of disease, poverty, and other considerations. Students were also responsible for completing a presentation on the Honduran healthcare delivery experience with a consideration of the disease states encountered. All students participated in the student presentations as both a learner and a presenter. Students received feedback from faculty related to their presentations to reinforce students’ ability to further develop cultural sensitivity and a more compassionate approach to patient care as suggested previously. The goal of our study was to understand how the experience met student expectations and the impact the medical mission APPE had on their empathetic and compassionate approach to patient care, which has not been previously assessed in the literature.
Methods
This study consisted of two surveys, administered to all students who were completing a medical mission APPE to Honduras. Pre-surveys were administered after orientation but prior to departure to Honduras and the post-survey was administered during the final week at the completion of the course. For survey design, school of pharmacy faculty completed a literature review using a Pub Med search to review previously published literature. Search terms included “international APPEs”, “medical mission”, and “APPE medical missions” [1-5]. While no pilot study was performed, a workgroup of faculty and experiential members who had previously precepted students in similar experiential courses drew on their experiences to help develop the surveys in conjunction with the literature review. Pre- and post-surveyquestions were developed by this workgroup to primarily assess changes in student perceptions based on their experiences using the online Qualtrics ® survey tool. Student participation was anonymous.
Surveys contained 22 questions in the pre-survey and 26 questions on the post-survey with the majority of questions appearing on both surveys. The post-trip survey contained additional questions to assess if students recommended future students study Spanish prior to the trip, if they recommended the course for future students, and if any personal illness was encountered that would prevent them from participation. Various question types were used and included multiple choice, a 5 point Likert scale, select all that apply and other question designs. Students were also given opportunities to provide short free text answers for certain items that required reflection. Topic areas assessed in the questions were related to how the student perceived healthcare in a developing country, poverty, communication, interdisciplinary care, and other key areas. The pre-and post-trip surveys were compared and evaluated to understand the impact the experience had on student expectations, perceptions, their empathetic approach to patient care, and to assess achievement of course objectives. Due to the limited number of students that can be assessed, the study would not have power to calculate statistical significance, but the authors feel that the importance of these type of courses on the student learning experience is important to share nonetheless. This study was approved by the Marshall University IRB (IRB Net ID# 1256665-1)
Findings
The student response rate for those completing the course/experience was 100%. Respondent numbers were n=18 pre- and n=12 post-trip. The number of pre-trip survey respondents is higher because some students completed the pre-trip survey and were not able to complete the in-country experience because their trip was cancelled prior to departure due to rioting and protests in Honduras and student safety concerns. Students unable to complete the experience were not administered a post-trip survey. Due to the anonymous nature of the survey, we were unable to separate those student’s responses.
Students results in the pre-trip survey, 28% (n=5) had not travelled internationally before this APPE while 72% (n=13) had travelled out of the country at least once. While some students had travelled internationally, only 11% (n=2) of students had ever travelled as part of a medical mission trip prior to this course.
Students who registered for the course indicated their perceptions of why they thought completing this course would be beneficial to their professional development. After the trip, students reflected on the experience and their perceptions at that point. Results from the two surveys are compared and displayed in Table 1. Survey results indicate that before taking this course, “a desire to help others” was the most common perception of what students would gain from this learning experience. Post-course, survey results indicate the biggest perceived benefit the students gained was “related to helping others”.
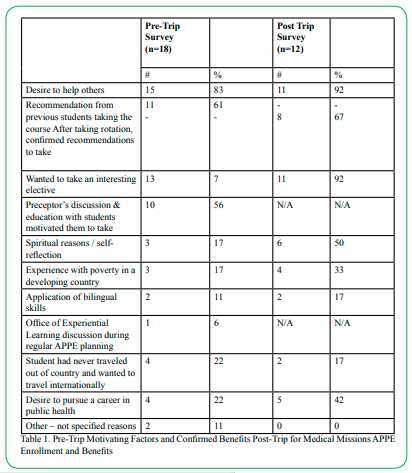
Table 1: Pre-Trip Motivating Factors and Confirmed Benefits Post-Trip for Medical Missions APPE Enrollment and Benefits
In the survey, we assessed student perceptions related to communications in this type of setting. Since the official language in Honduras is Spanish and most students visiting the country were only fluent in English, the survey attempted to assess perceptions pre- and post- related to communication challenges for health care providers [9]. Students were asked on the pre-trip survey to identify how many patients they perceived would be able to communicate in English. Eleven students (61%) believed as many as half of the patients would be able to speak some English. Post survey, results indicated that few patients were able to communicate in English with providers. Only 17% (n=2) of attendees indicated they spoke at least moderately fluent Spanish, which indicated a potential challenge. The rest of the participants indicated they were only fluent in English or other unrelated languages. The students not fluent in Spanish did not plan to rely on an interpreter or electronic translation. A majority of students indicated they planned to study Spanish prior to their departure. In actuality, post survey results indicated students who were not moderately fluent in Spanish required the use of a translator while providing care. No internet access was available in the rural environment to facilitate use of electronic translation tools. Post-trip, 100% (n=12) of respondents indicated students in future trips should study Spanish prior to the trip.
Prior to the trip, students were also surveyed on perceptions related to the Honduran healthcare system and related living conditions. The majority of students, perceived healthcare was provided in a similar manner as in the United States by government funded programs or private health insurance. Prior to the trip, 83%(n=15) of students believed patients would travel greater than five miles to receive healthcare provided by the clinic. Post-experience, students indicated that a majority of patients did not have access to transportation (individual or public), resided in a very rural environment, and without the medical mission providing care near the patients, and would have travelled greater than five miles for care. Students and faculty noted that many patients relied almost entirely on services provided by the clinics for their healthcare.
Students were also asked questions on the survey related to poverty. In terms of basic living conditions like sanitation in Honduras, half of students believed less than 25% of patients would have running water and half of students believed 26-50% would have running water. Post-trip perceptions, 83% of respondents confirmed the majority of the rural patients served (>50%), struggle on a day-to-day basis with items such asbasic sanitation including obtaining clean drinking water. Residents had to walk miles and boil water to ensure adequate potable water. Reflection statements indicated that seeing the challenges rural Hondurans faced in obtaining clean drinking water was a new experience for some students. Students had never experienced this level of poverty and the associated challenges. On the post survey and during student reflection, students discussed marked changes in their perceptions, empathy, and importance of providing compassionate care.
Survey results demonstrated (select all that apply question) this experience was life changing for them 67% (n=8) and/or changed their perceptions/empathy towards patients as a healthcare provider 83% (n=10). Students were asked a “select all that apply to your applicable situation” question and the majority of students 75% (n=9) indicated they found the experience of helping others rewarding as one of the main benefits. A representative sampling of student comments are displayed in Table 2. Finally, students over whelmingly responded to the survey they strongly agree future students should take this course 92% (n=11), or somewhat agree students should take this course 8% (n=1).
Discussion
Measuring how students perceive medical mission APPEs and how it changes their professional approach to care has not been widely discussed or assessed in the literature. Represented by student feedback, we found that students gained valuable experiences (see table 2) and were able to apply knowledge of travel medicine, patient assessment, and acute and chronic care in these courses. Students demonstrated in the survey results, many benefits in their professional development. Marked changes were noted in empathy or provision of care to those in poverty, spiritual reflection, and in desire to pursue a career in public health or a related field. Students experienced some of the many challenges faced by health care providers in communicating with those of other cultures and languages. Students did not perceive communications to be a significant barrier prior to the experience, but demonstrated in the post-trip reflections the many challenges faced by clinic staff in regards to communications, including lack of Wi-Fi, reliance on a nonmedical interpreter, illiteracy, and limited time to spend with each patient. Students can apply lessons learned in future encounters with patients from another culture or with limited English proficiency.

Table 2: Student Comments Regarding International Medical Mission APPE as Related to Being a “Life-Changing” Experience
Prior to the trip students were asked questions related to the healthcare systems in Honduras. Survey results demonstrated students had minimal exposure to other international health care systems and a general lack of understanding of the Honduran health care system. After the trip, many reflected on the post-trip survey regarding the inadequate health care infrastructure seen in Honduras. Students were surprised to discover the limited number of providers, minimal funding, and disparities. Students noted that this often results in inadequate provision or lack of care provided to patients. As a result there is an increased need for medical mission clinics to help fill the void in care for these patients. Survey results demonstrated that influences from the trip may alter student’s perceptions about the world, international health care, empathy toward others, and care to those who are less fortunate.
Student’s completing this course had extensive experiences in managing patients with SDOH by course design. Students were able to directly observe populations with a deficiency of potable drinking water, poverty, lack of health care, and an inadequate transportation system. Students developed a more appreciative and empathetic approach to care of patients as a result to these experiences as noted in the post course reflections.
Overall, our study demonstrates that these experiences were life changing, altered students approach to care to be more empathetic, and proved to be an overall positive impactful experience for students in their professional development. Students noted that their perceptions and approach to care would be different moving forward with a majority stating that they wanted to do more in the public health sector and felt these type of experiences would be beneficial to other students in the future.
Survey results and reflections obtained demonstrated that those without anyprevious exposure to healthcare in a developing country had marked changes in perceptions and empathy. Survey participants indicated the experience substantially increased their “desire to help others”. We believe that this is an indication that students will approach the care of patients living in poverty more empathetically post-medical mission APPE experience. These skills will be important as students develop their own pharmacy practice and approach to taking care of patients. This is especially important with patients who may have certain SDOH, live in poverty, or have other health disparities.
There are several limitations to this study. The overall total number of students able to complete this APPE course is limited due to group lodging space in Honduras, travel funds, size of the interdisciplinary group, and ongoing travel restrictions. This study was completed over a two-year period with two separate trips and the experiences were not identical. In addition, some students were unable to complete the course due to in-country safety concerns as previously noted. Due to ongoing COVID travel restrictions, this course remains on hold and we were unable to get a larger sample size.
Summary
Results of this study support the value of exposing students to healthcare in a developing country as an APPE course. Students streng thened their knowledge and skills related to providing care to those in poverty, addressing barriers to communication, and enhanced their empathetic approach to care as part of the experience. Currently, students can only complete medical mission or international healthcare experiences as part of our program in the experiential portion of the curriculum. It is completed as part of an elective APPE as required by ACPE for all international experiences [10]. Students subjectively confirmed value of the course by giving comments that this course should be required for all healthcare professionals. In general, responses indicate this was a life-changing experience, which will affect their approach to providing care in an empathetic manner.
Due to the ongoing COVID-19 pandemic, many of these life-changing courses have been suspended with long-term suspensions possibly lasting into a third academic year. Considering these ongoing suspensions of travel and funding, the viability of these courses are threatened. Experiential consortiums and schools of pharmacy should explore ways to partner and ensure continuation of these valuable experiences for students and patients in the future. Perhaps by working together we can preserve these experiences in the face of these barriers. The authors also realize due to travel expenses, funding, opportunity, and other factors beyond a student’s control, this would be an unrealistic experience to require for all students. However, responses from our study results reinforce the value and need for pharmacy programs to offer interdisciplinary medical mission APPE opportunities to students interested in pursuing these life-changing experiences.
Competing interests:
The authors report no conflict of interest.
References
Alsharif, N.Z., Dakkuri, A., Abrons, J.P., et al. (2016). Current Practices in Global/International Advanced Pharmacy Practice Experiences:Home/Host Country or Site/Institutional Considerations. American Journal of Pharmaceutical Education;80(3):Article 38.View
Brown, D.A., Ferrill, M.J. (2012). Planning a pharmacy-led medical mission trip, part 3: development and implementation of an elective medical missions advanced pharmacy practice experience (APPE) rotation. Ann Pharmacother. 46(7-8):1111- 1114. doi:10.1345/aph.1Q735.View
Dornblaser, E.K., Ratka, A., Gleason, S.E., et al. (2016). Current Practices in Global/International Advanced Pharmacy Practice Experiences: Preceptor and Student Considerations. American Journal of Pharmaceutical Education.80(3):Article 39.View
Johnson, K.L., Alsharif, N.Z., Rovers, J., et al. (2017). Recommendations for Planning and Managing International Short-term Pharmacy Service Trips. American Journal of Pharmaceutical Education;81(2):Article 23.View
Smith, J.N., Phan, Y., Johnson, M. et al. (2018). Describing pharmacy student participation in an international interprofessional medical mission trip as part of an advanced pharmacy practice experience (APPE). Currents in Pharmacy Teaching and Learning. (10):940-945.View
Steeb, D.R., Overman, R.A., Sleath, B.L., et al. (2016). Global Experiential and Didactic Education Opportunities at US Colleges and Schools of Pharmacy. American Journal of Pharmaceutical Education;80(1):Article 7.View
Scott, D.M., Naughton, C., Haugen, K., et al. (2019). Study Abroad Course for Pre-pharmacy and Pharmacy Students to Learn About Global Health. American Journal of Pharmaceutical Education.83(8):Article 6866.View
Werremeyer, A.B., Skoy, E.T. (2012). A Medical Mission to Guatemala as an advanced Pharmacy Practice Experience. American Journal of Pharmaceutical Education.76(8):Article 156.View
Fact Sheet – Honduras. United States Department of State website. https://www.state.gov/u-s-relations-with-honduras/. Accessed March 3, 2020.View
Accreditation standards and guidelines for the professional program in pharmacy leading to a doctor of pharmacy degree. Accreditation Council for Pharmacy Education (ACPE) website. https://www.acpe-accredit.org/pdf/Standards2016FINAL.pdf. Accessed March 3, 2020View

