Journal of Public Health Issues and Practices Volume 6 (2022), Article ID: JPHIP-210
https://doi.org/10.33790/jphip1100210Review Article
Proposing an Educational Video: Preventing Airway Occlusion with Infants in Supported Sitting
Margaret L. Alston*, Malliga Jambulingam
Morgan State University, School of Community Health and Policy, Portage Hall, 4530 Portage Ave. - Room 302K, Baltimore, MD 21239. United States.
*Corresponding Author Details: Margaret L. Alston, PT, PhD, Assistant Professor, Morgan State University, School of Community Health & Policy, Portage Hall, 4530 Portage Ave. - Room 302K, Baltimore, MD 21239. United States.
Received date: 24th August, 2022
Accepted date: 24th September, 2022
Published date: 26th September, 2022
Citation: Alston, M. L., & Jambulingam, M., (2022). Proposing an Educational Video: Preventing Airway Occlusion with Infants in Supported Sitting. J Pub Health Issue Pract 6(2): 210.
Copyright: ©2022, This is an open-access article distributed under the terms of the Creative Commons Attribution License 4.0, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Introduction
Sudden Unexpected Infant Death (SUID) includes the full spectrum of all infant death causes, which include “Determined” causes [e.g. Sudden Infant Death Syndrome (SIDS) at 42% and Accidental Suffocation and Strangulation at 24%], as well as “Undetermined” causes at 34% [1]. Literature is replete with studies that address the risk factors associated with SIDS, accounting for at least 42% of infant mortality [1]. Scarce to find, however, is public health education or learning opportunities that address the mechanism of brain injury and death by Positional Asphyxiation (PA). Better yet, in the current day of popular social media platforms and cell phone apps, there should be readily available video education on the topic where the focus is on PA risk factors and prevention. Viewing should be required of new parents and caretakers, as well as to health professionals, including pediatric clinical trainees who specialize in infant care. Other suggested locations for viewing would be hospital postpartum delivery suites and pediatric waiting rooms.
The accidental but preventable phenomenon of PA gives rise to the annual occurrence rate of 2.8 – 3.0% (98-105 deaths) in healthy infants who have no pre-existing medical conditions, including prematurity. They die from SUID primarily in car seats, accounting for 69% of deaths in sitting devices [1]. Webster’s Dictionary defines PA as, “A condition of deficient oxygen supply to the brain and body which occurs when a person’s physical position prevents normal breathing.” Each tragic occurrence is first suspected, then largely confirmed by a combination of investigative reports and the absence of gross or observable findings from post-mortem autopsy--like tissue injury from traumatic injury or inflammatory changes. Additionally, there would be no recorded or known history of a pre-existing medical condition. Given these factors, post-autopsy typically confirms the cause of death as “Undetermined or Unknown.” Perhaps the combination of the low incidence rate of PA and “Undetermined” autopsy reports cause this mechanism of infant mortality to be an “unsung” category of SUID, thus remains in obscurity with respect to disseminated public health education.
Turning focus to the critical developmental period of young infants –that concerns the morphology of the spine, head and neck alignment, upper back strengthening, and pliable upper airway vulnerability, PA occurs most often in young infants who are less than 5 months of age.
While PA is less common than other causes of SUID, the mechanism by which the infant’s airway becomes occluded is scarcely brought forth by public health authorities or illustrated. One preventable infant death due to PA, however, is very much worth the attention I hope that the advocacy for available video education receives.
If the etiology of PA was clearly illustrated by a reasonably short video and was easily available to the public, new parents and caretakers of young infants would be better equipped to make wise decisions and consistently practice proper positioning approaches when situating especially young infants in all sitting devices.
Equally important, insightful decisions would likely be made concerning their choices of caretakers for their infant(s). Given the higher probability of accidental positioning errors among young and less mature caretakers, informed parents would opt to leave their infant(s) with a more mature, more responsible, and compliant caretaker who too has been educated about the risk factors of PA and proper positioning in sitting devices.
It is important to highlight that researchers who study PA fatalities in car seats concur that there is no increased risk of SUID for healthy infants appropriately transported in vehicles when the car seat is properly used for transportation only, and when the infant is safely reclined and secured (Figure 1). In other words, SUID occurring in car seats is very uncommon among the population of normal infants when the infant is properly reclined and secured [2]. Note that the infant is properly reclined to ~45o to offset gravitational forces, thus protecting the normal airway patency.
For decades, many well-respected pediatric authorities (e.g. United States Centers for Disease Control and Prevention; American Academy of Pediatrics; US Consumer Product Safety Commission: Children’s Products, etc.) have published guidelines for proper use of infant sitting devices [3-5].
Despite written instructions and guidelines for proper use of car seats by pediatricians, public health experts, and other well-respected authorities of pediatrics, such as The American Academy of Pediatrics (AAP), hundreds of young infants are subject to the risk of PA daily – if there is an occasion that improper positioning including the infant’s pelvis being in a posterior versus neutral tilt and/or belt restraints are not snuggly secured. Thus, the more occasions and the more time that young infants are in car seats, the greater the opportunity and probability that sustained neck flexion (chin or chest) position could occur, lending to the folding of the upper airway on itself causing the infant to suffer ischemia (reduced oxygenation) or hypoxia (absent oxygenation).
According to an observational study entitled “Use of Seating Devices of Infants Too Young to Sit,” where surveys focused on use patterns of sitting equipment by parents of infants less than 5 months, outcomes revealed that in their sample size of 187, 94% or 176 infants spent an average of 5.7 hours per day in their car seats [4]. These findings seem to imply that car seats are being used to position infants in places other than in vehicles. In the studies cited above, researchers concur that when infants are seated or positioned incorrectly, infant safety is notably compromised [5-10].
Use of Car Seats in the United States
In the web-based article, “Do You Know the 2020 USA Car Seat Laws for Your State and States You Visit?” it outlines the car-seat laws for each state categorized by region [11]. Interestingly, most all states highlight: the age range for required rear-facing or front-facing, as well as height and weight requirements for booster seats, etc. None, however, address the need or importance of adequate reclining of infants. It is therefore very important for caretakers to follow manufacturer instructions which address the proper reclining method. It is also very important for caretakers to revisit the manufacturer’s instructions as the infant ages through 12 months, since proper positioning requirements change with the infant’s overall size and developmental stage.
When car seat instructions are not followed and out-of-car uses are the case, infants can succumb to accidents like: falling from a car seat that is placed on an elevated surface, flipping over the sides of the device, or slipping under loose strap/belts to become hung by the neck and strangled to death [6,10]. Given these scenarios, “Determined” becomes the categorical cause of death given autopsy findings of: head trauma, suffocation, or strangulation respectively [6-9].
Incidence Rates of Positional Asphyxia in Infants Improperly Secured in Car Seats
In the comprehensive 2019 study by Liaw et al., whose aim was to analyze the characteristics of 11,779 sleep-related infant deaths, 348 or 3% occurred in sitting devices [9]. The majority of infants who died in a sitting device (219 of 348 or 69%) died in a car seat. The remainder (129 or 31%) died in bouncers, swings, strollers, or other sitting equipment [1,9].
The 3% of deaths that occur in sitting devices are consistent in other published work [8,10]. The grand majority of the 3% comprise approximately one-half of infants who: died in a car seat (vs. stroller), were less than 5 months (not including prematurity); were located in non-traveling settings; and were suspected of dying from PA with “Unknown” or “Undetermined” causes of death [6-9].
Regarding upper airway occlusion (not caused by equipment strap or belt accidents), specific developmental and anatomic factors shall be illustrated in the proposed video to best understand what the critical requirements are to maintain airway patency. Whether the young baby is in the arms of a parent/caretaker or on their lap, all positions initially require physical support of the head and neck, thereby protecting full airway patency for normal breathing (Figures 2 & 3).
Methods
As the expression goes, “A picture is worth a thousand words.” Proposed is the production of a technically-sound life-like video which depicts the developmental and anatomical changes that ultimately render the older infant less susceptible to PA.
The first of a two-part methods approach includes surveying and illustrating peer-reviewed and published textbook materials that address the three concurrently occurring factors that put young infants at risk for PA in upright sitting.
Three Anatomical and Developmental Factors Combines to Cause Positional Asphyxia:
The triad (3) of key anatomical and developmental factors that when superimposed or occurring together make especially the young (<5 mos. of age) infant’s airway vulnerable to airway obstruction when seated in the upright or vertical position. They are:
1. The C-Shaped Rounded Spine of the Young Infant
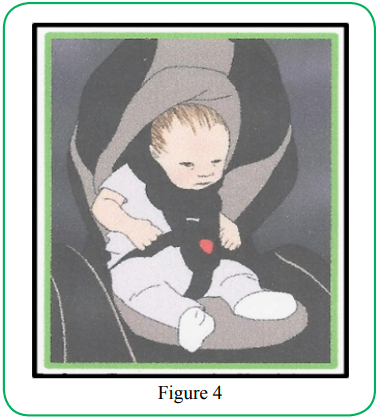
The C-shaped rounded spine (in the sagittal plane or when viewed from the side) along with a posteriorly tilted pelvis (Figure 4).
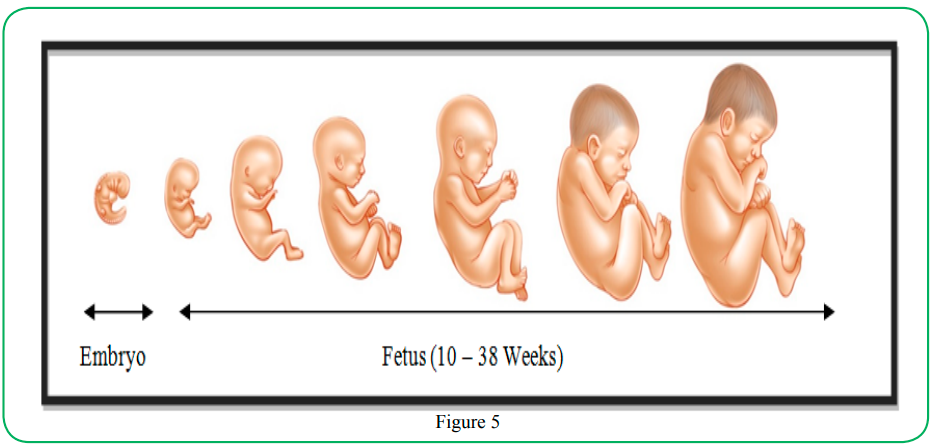
With normal prenatal development, the embryonic spine is C-Shaped in the sagittal plane (Figure 5), [11] where the sagittal plane divides right and left sides, as one of three spatial planes. The C-shaped spine persists from the fetal period (10 weeks gestation) through birth and very early infancy (1-2 mos.) [11]. Additionally, the rounding of the spine at the rump contributes to the spine’s C-shape in the fetal stage –which still persists through birth and early infancy, which is in part due: to the winged-shape of the pelvis [12] and the rounding external forces directed to the spine from the mother’s strong uterine and abdominal walls.
2. Inadequate Head Control
Since the young infant’s head is approximately 25-30% the size and weight of the full body, along with underdevelopment or weakness of posterior neck and upper back musculature, the infant struggles to control its head position up against the downward force of gravity.
The mechanical vulnerability of the head position to the effects of gravity, along with the soft histologic tissue properties of the larynx within the upper airway, cause the infant’s upper airway to be very much at risk for folding –like that of a straw that is bent in half.
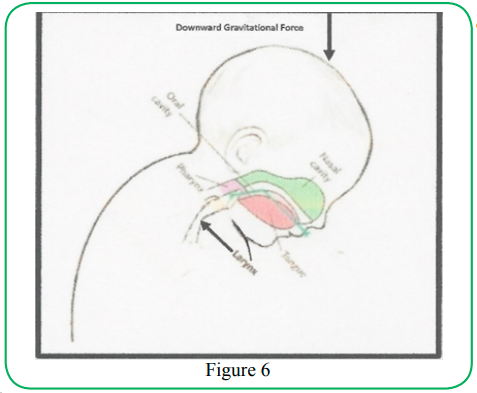
Contributing to its risk to become occluded is the superior location of the laryngeal complex at the level of the lower jaw or mandible, where neck flexion takes place (Figure 6).
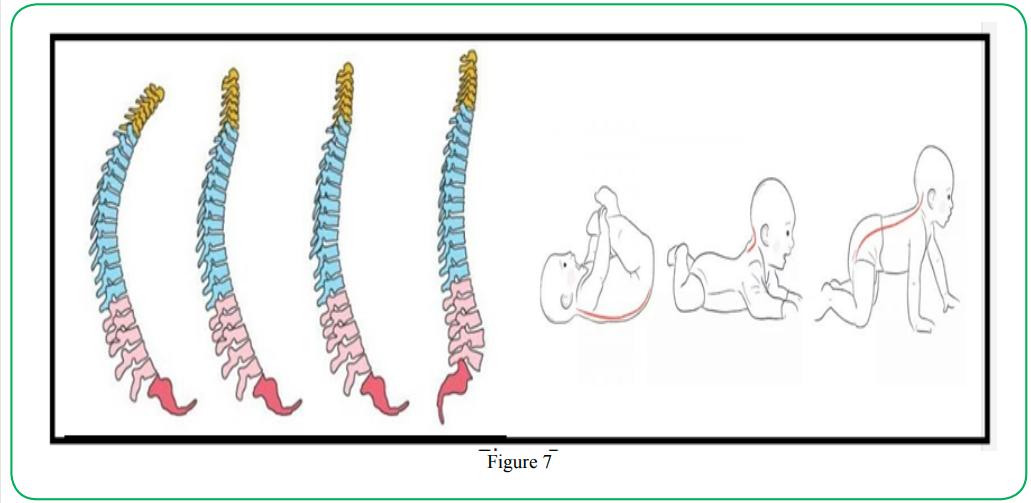
By the age of 3 months the of neonatal vertebral spine transforms from a C-shape to the more mature S-shape [13] (Figures 7), maturation of the laryngeal complex and strengthening of the upper make the aging young infant less at risk for PA, once they are older than 4 months.
3. Upper Airway Properties
The third developmental factor specifically addresses the laryngeal complex of the upper airway. Its high (superior) location in the neck-- which approximates the C3 and C4 cervical vertebrae levels, along with its cellular pliability, and its conical shape puts the larynx, in the upper respiratory tract, at risk for occlusion when there is maximal and sustained neck flexion. The cellular make-up of the larynx is diversified, due to its varying degrees of elastic tissue that span the length of the organ. Additionally, the 7 cartilaginous structural regions that provide its composition, and its ellipsoid or conical shape contribute to its complexity [14].
The significance of its conical shape is that the least stable or most pliable aspect is closest to the superior aspect of the upper airway-- close to the infant’s jawline where occlusion occurs. In contrast, the most stable or least pliable aspect is distal or furthest away from the top of the airway, near the transition to the trachea, the anatomical connection to the lung’s main bronchus.
The Oct. 2017 article entitled, “The Anatomy of the Pediatric Airway: Has our Knowledge Changed in 120 Years” [14] confirmed that the laryngeal organ complex has the three main functions: safe swallowing (given its epiglottal folds) at the upper end, sound production (given the V-shaped vocal cords), and respiration (air exchange to/from the lungs). The various cartilaginous types are mucosa-covered, highly deformable and flexible [14] and able to with stand repeated bending and rebounding dynamics, just as other bodily structures made of elastic cartilage are capable of.
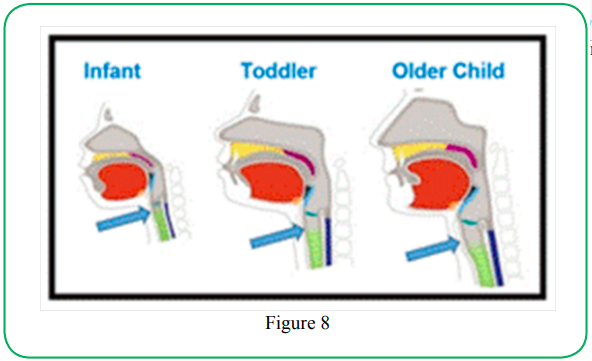
It should be reiterated that the most vulnerable developmental stages of the larynx are greatest in the young infants (less than 5 mos.), which is coincident with the population of infants who succumb most to PA in the upright seating position. In the discussion of developmental maturation, there becomes greater histologic stability (less flexibility) of the upper airway as the infant ages to young childhood [15]. For example, a 3-year-old child can better withstand deformable forces of neck flexion because of their more mature histologic or tissue make-up, and additionally since the laryngeal complex in the upper respiratory track shifts to a lower position by toddlerhood (Figure 8) [16].
Developmental Factors that Protect the Aging Infant’s Airway
Upper back and head control helps to protect the airway patency in the aging young infant. Natural nurturing often incorporates goal-directed handling by parents and caretakers, which builds in opportunities for the infant to move against gravity in various positions on a regular daily basis.
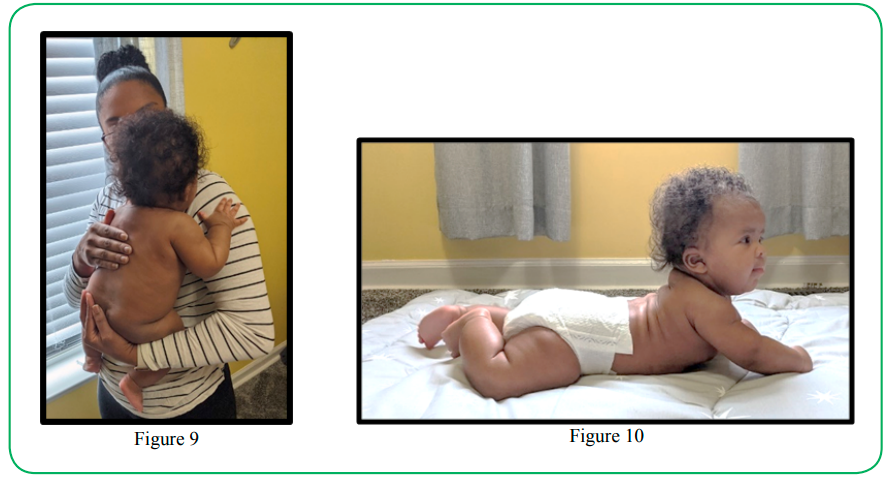
Position recommendations utilize simple illustrations involving the mechanical inter-relationships between the spine, hips, and pelvis that together impact the position of the head and neck –critical in the discussion of airway patency or respiration safety. When the infant is active against gravity, progressive strength balance of flexor and extensor muscle groups about the neck and upper back evolve, first beginning when the young infant is regularly supported against the chest of an upright caretaker (Figure 9), as well as when active in supervised “tummy time” (Figure 10).
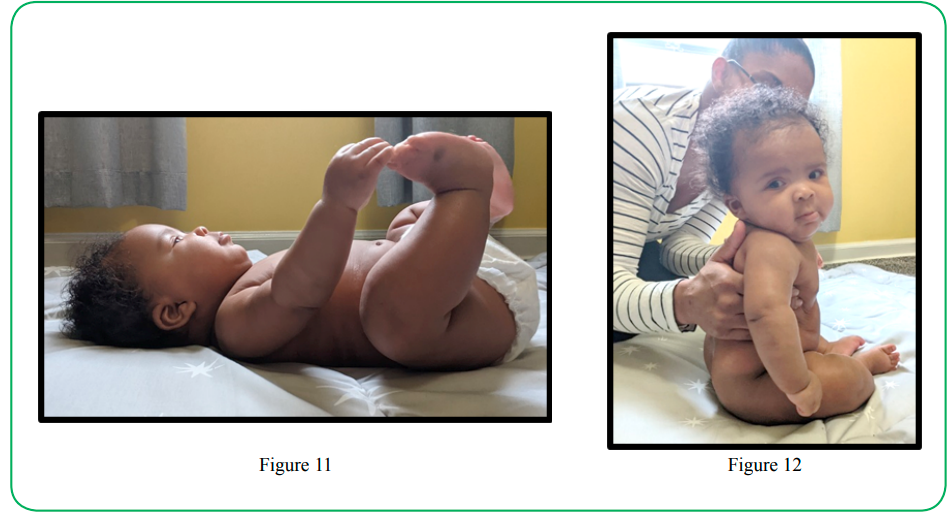
Around the 4th month of age, active muscle efforts around the spine, neck, chest, and abdomen occurring from the supine and prone positions assist with midline regard while right/left symmetry emerge (Figure 11). This phase of development is key for the emergence of independent antigravity head control (Figures 7 & 8) [17]. Centered head control is assisted when the forearms push against a supportive surface (Figure 7) [18]. In keeping with the normal developmental progression, core or axial component parts (e.g. head, neck, and spine with trunk) mature before the more distal or peripheral segments.
In the infant who is being handled and mentally stimulated from all positions when alert, the axial development of the muscles about the neck and upper trunk become very strong and balanced, capable of moving various segments of the body against the downward force of gravity within the first 4-5 months. The importance of this order of developmental events is that the older infant (> 4 mos.) can better steady its head upright and is less vulnerable to uncontrolled neck flexion and airway constriction (Figure 12). Upper airway occlusion is therefore much less at risk in the older infant who is alert and in supported sitting (Figure 12).
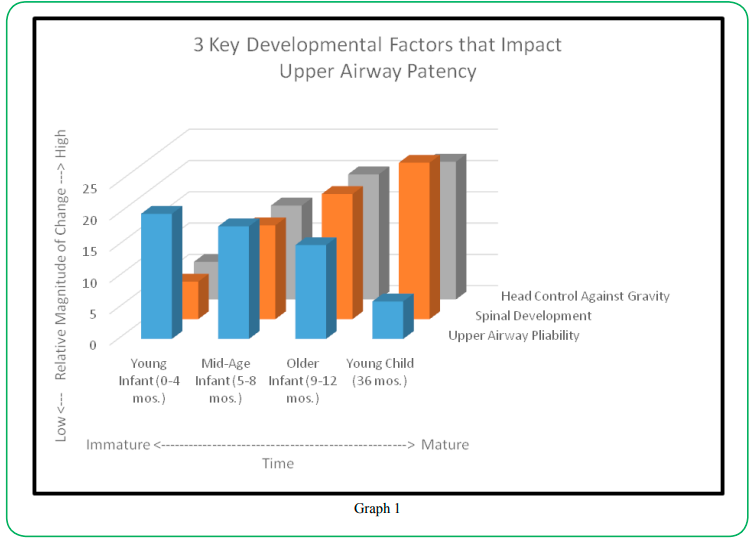
It should be noted that the articulated interrelated factors causing younger infants to be most vulnerable to PA compared to older infants and young children are enumerated and illustrated in Graph 1. As seen, there is an indirect relationship between an infant’s age and the magnitude of elasticity or deformability of the upper airway.
As the baby ages, progressive maturation of the laryngeal complex which includes decreasing pliability, takes place which helps to protect the airway from the risk of deformable forces. In contrast, spinal curve maturation and head control have a direct relationship with the aging infant. They increase and mature together.
The second phase of the two-part Methodology will collect quantitative data from a minimum of 200 consenting first-time parent participants --using a 15-question Likert Scale pretest/posttest design, where the video instruction would follow the pre-test.
Student T-Testing of the one-tailed data set would measure the extent of learning by the targeted sample with a set confidence level of 95%, creating a significance value of 5% such that the null would be rejected.
Results
With use of the pre-video and post-video, where the questions are identical, the change in scores per participant would hopefully but likely indicate that the extent of learning was significant at least at the p ≤ .05 level. If the p-value is found to be less than the significance value, the investigators would be sure that true learning would occur at least 95% of the time, and that any random learning would occur less than 5% of the time.
Discussion
Developmental and position-based evidence reveals that the immature conditions of the cervical spine shape; muscular weakness about the neck and upper back; cellular properties, location, and shape of the upper airway all together contribute to the vulnerability for upper airway occlusion in especially young infants when the head falls forward and the neck is maintained in flexion. This high-risk life-threatening scenario is known to be precipitated by improper vertical-sitting positioning (Figure 4).
Of course, the true value or merit of the video instruction comes with a built-in assumption that the learning outcome would translate to improved or consistent safe positioning practices by at least new parents and caretaker video-viewers, thus helping to lower the incidence rate of SUID by PA.
Given such an outcome, the video could be introduced as a public health teaching tool and be added to the library of instructional videos currently shown in hospital post-partum suites, in outpatient offices of pediatricians, neonatologists, and obstetricians, on transportable DVD players used by doulas and midwifes in home settings, social media platforms, as well as be available on cell phone apps. Such a campaign would be justified.
Recommendations for Infant Airway Protection:
Though proper handling of infants most always occurs instinctively or naturally. However, due to the existing 3% incidence rate of PA, heightened awareness about the importance of neutral alignment of the infant’s head and neck by caretakers is indicated. Additionally, it must be emphasized that follow the manufacturer’s seating device instructions, which includes adjustments as the infant ages, is essential.
Car Seat Positioning Recommendations for PA Prevention - And Proposed Video Highlights
1. Semi-recline the backward-facing car seat to approximately 40- 45 degrees for all infants (0-12 mos.) whether awake or asleep, while ensuring that the head and neck alignment is in neutral, checked in all 3 spatial planes. That is, ensure that the neck is not in: forward flexion, backward extension, extreme rotation (right/left), or extreme side bending(right/left) (Figure 1).
2. Following these guidelines will best ensure that neck flexion will not occur –whether the infant is awake or asleep, and that neutral alignment of the head and neck will be preserved to best ensure normal airway patency
3. The adequate angle of recline will differ slightly among infants of varying ages. The ultimate aim is to ensure neutral alignment of the head and neck to protect the upper airway. Even when a tilt gauge is built into the sitting device, normal head and neck alignment will be ultimately visually assessed.
4. Have knowledge of the infant’s age and refer to the device’s instructions with regularity --since the age will correlate with proper use and adjustment recommendations by the car seat’s manufacturer.
5. Soon after purchase of the device, register the device online, including an active email address, so that Inbox notification of any consumer alerts or recalled parts/devices can occur
6. When choosing an infant in a car seat for proper positioning:
• Ensure that the seat width allows for adequate spreading of the thighs with outward rotation of the hips so that the pelvis can be maintained in neutral (e.g. not tilted backward or forward)/ (Figure 1; Position B). This position helps the spine to maintain the mature elongated S-shape, allowing the baby to control its head in neutral and in midline to withstand uncontrolled neck flexion.
• Parents and caretakers should take care to use car seats and other sitting devices for their original and recommended use, since doing otherwise can introduce significant safety risks to the infant, which could result in injury or SUID [19].
• All sleeping infants should be removed from their car seat or other sitting devices as soon as is plausible and laid down on their back (e.g. infants less than 7 months) in a safe-sleep crib, bassinet, transportable bed, etc.
Suggested Sources of Information About Infant Safety and Equipment:
a) https://www.cdc.gov/motorvehiclesafety/child_passenger_ safety [CDC: Motor Vehicle & Child Passenger Safety]
b) https://www.cdc.gov/injury/features/child-passenger-safety [CDC: Child Passenger Safety Guidelines]
c) https://www.nhtsa.gov [National Highway Traffic Safety Administration]
d) https://www.safekids.org [Safe Kids Worldwide]
e) https://www.nsc.org [National Safety Counsil]
f) https://bestcarseathub.com/blog/usa-car-seat-laws-2020 [2020 USA Car Seat Laws for Your State]
g) https://www.cpsc.gov [Consumer Protection Safety]
Competing Interests:
The authors assert that there are no conflicts of interest.
List of Abbreviations
AAP - American Academy of Pediatrics SIDS - Sudden Infant Death Syndrome SUID - Sudden Unexpected Infant Death PA - Positional Asphyxiation/Asphyxia
Acknowledgements
* Aaliyah and Parents (Prishani & Justin) * Sienna and Parents (Lauren & Chris) * Jay Alston (Freelance Artist: Bel Air, MD)
References
National Center for Health Statistics. https://www.cdc.gov/nchsView
Batra, E., Midgett, J. & Moon R. (2015). Hazards Associated with Sitting and Carrying Devices for Children Two Years and Younger. The Journal of Pediatrics, 167(1): 183-187 https:// doi.org/10.1016/j.jpeds.2015.03.044View
United States Center for Disease Control and Prevention. https://www.cdc.gov/grand-rounds/pp/2018/20181023-sudden-infant-deathView
The American Academy of Pediatrics. https://www.aap.orgView
United States Consumer Products. https://www.cpsc.govView
Bamber, A., Pryce, J., Ashworth, M., & Sebire, N. (2014). Sudden Unexpected Infant Deaths Associated with Car Seats. Forensic Sci Med Pathol, (10): 187-192. View
Cote, A., Bairam, M., Deschenes, M., & Hatzakis, G. (2008). Sudden Infant Deaths inSitting Devices. Arch Dis Child (93): 384-389. DOI: 10: 1136/adc.2007.119180View
Freyne, B., Hamilton, K., Garvey, C., Matthews, T., & Nicholson, A. (2014). Sudden Unexpected Death Study Underlines Risks of Infants Sleeping in Sitting Devices. Acta Paediatrica, 103(3): 130-2.View
Liaw, P., Moon, R., Han, A., Colvin, J. (2019). Infant deaths in sitting devices. Pediatrics, 143 (6):1-7. https://doi.org/10.1542/ peds.2018-2576View
Kassa, H., Moon, R., & Colvin, J.D. (2016). Risk Factor for Sleep-Related Infant Deaths in In-Home and Out-of-Home Settings. Pediatrics, 138(5): 1-6. View
Bess, S., Varma, V. (2011). Embryology and Anatomy: Spine/ Spinal Cord, Springer-Verlag Berlin Heidelberg.View
Delaere, O., Dhem, A. (1999), Prenatal Development of the Human Pelvis and Acetabulum, Acta Orthopaedica Belgica, 65(3): 255-60.View
Gerber, R.,Wilks, T., Erdie-Lalena C. (2010). Developmental Milestones: Motor Development. Pediatrics in Review, 31(7): 267-277. DOI: https://doi.org/10.1542/pir.31-7-267.View
Holzki, J., Brown, K., Carroll, R., Coté, C. (2018). The Anatomy of the Pediatric Airway: Has Our Knowledge Changed in 120 Years? A Review of Historic and Recent Investigations of the Anatomy of the Pediatric Larynx. Pediatric Anesthesia, 28(1): 13-22. DOI: 10.1111/pan.13281.View
Yonekawa, S., Fukunaga, H., Umeno, H., Mori, K., Nakashima, T. (2000). Subglottic Airway Becomes Stable with Age in the Human Infant Larynx. Acta Oto-Laryngologica, 120(3): 444- 449. DOI:10.1080/000164800750000711View
Xi, J., Si, X., Zhou, Y., Kim, J., Berlinski, A. (2014). Growth of Nasal and Laryngeal Airways in Children: Implications in Breathing and Inhaled Aerosol Dynamics. Respiratory Care, 59(2):263-273.DOI: https://doi.org/10.4187/respcare.02568.View
Alexander, R., Boehme, R., Cupps, B. (1993). Normal Development of Functional Motor Skills: The First Year of Life. Hammill Institute. View
Siddicky, S., Bumpass, D., Krishnan, A., Tackett, S. McCarthy, R., Mannen, E. (2020). Positioning and Baby Devices Impact Infant Spinal Muscle Activity. Journal of Biomechanics, (7)104. https://doi.org/10.1016/j.jbiomech.2020.109741.View
Callahan, C. & Sisler, C. (1997). Use of Seating Devices in Infants Too Young to Sit. Arch Pediatr Adolesc Med, 151(3): 233-235. DOI:10.1001/archpedi1997.02170400019004.View