Journal of Public Health Issues and Practices Volume 10 (2026), Article ID: JPHIP-252
https://doi.org/10.33790/jphip1100252Case Report
Beyond the Walls: A Study of Community Citizenship Processes and Results in Industry-Leading Healthcare Organizations
Andrew L. McCart, PhD, FACHE
Associate Professor, Department of Nutrition and Health Care Management, Beaver College of Health Sciences, Appalachian State University, Boone, NC 28608, United States.
Corresponding Author Details: Andrew L. McCart, PhD, FACHE, Associate Professor, Department of Nutrition and Health Care Management, Beaver College of Health Sciences, Appalachian State University, Boone, NC 28608, United States.
Received date: 20th September, 2025
Accepted date: 20th February, 2026
Published date: 23rd February, 2026
Citation: McCart, A. L., (2026). Beyond the Walls: A Study of Community Citizenship Processes and Results in Industry Leading Healthcare Organizations. J Pub Health Issue Pract 10(1): 252.
Copyright: ©2026, This is an open-access article distributed under the terms of the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited.
Abstract
This study examines two decades of nationally recognized healthcare organizations in the United States that earned the nation’s highest awards for performance excellence in healthcare delivery between 2005 and 2025. Using a structured qualitative document analysis design, the review synthesized publicly available award documentation, government reports, and peer-reviewed healthcare management literature to identify recurring organizational processes and measurable results associated with high-performing, community-engaged health systems. Data were extracted using a standardized abstraction template capturing organizational context, strategic management practices, community citizenship initiatives, and reported performance outcomes. A directed content analysis approach was used to code evidence into thematic domains aligned with performance excellence constructs and population health orientation, followed by cross-case synthesis to compare patterns across organizations and time periods. Findings indicate that honorees consistently aligned mission, strategy, and operations with community engagement and measurable quality and safety goals. Across cases, organizations extended impact beyond hospital walls through community benefit investment, social determinants of health initiatives, workforce pipeline development, and cross-sector partnerships, with reported improvements in clinical outcomes, patient experience, workforce engagement, and financial sustainability. Results suggest that high-performing systems operationalize community citizenship as a strategic capability supported by integrated management systems and continuous measurement, offering transferable lessons for health systems seeking to strengthen population health alignment and organizational performance.
Keywords: Healthcare Quality Management, Community Engagement, Organizational Excellence, Performance Improvement, Population Health, High-reliability Organizations
Introduction
Over the past twenty years, a select group of U.S. healthcare organizations has earned the nation’s highest honors for performance excellence in healthcare delivery. These awards formally bestowed by the U.S. President as national awards for quality—recognize hospitals and health systems that demonstrate outstanding leadership, patient outcomes, innovation, and community impact [1]. This review examines how award-winning healthcare organizations (2005– 2025) have aligned their mission and strategy with quality goals, implemented community programs to improve public health, and achieved measurable impacts in care quality, equity, and innovation [2].
Drawing on award program documentation, government reports, and healthcare management sources, this paper highlights best practices spanning the past 20 years. Notably, the findings are balanced across the entire period, showing that early pioneers (mid-2000s) and recent recipients alike embraced similar core principles [3,4]. Each section below, Introduction, Mission and Strategy, Community Programs, Measurable Impacts, Discussion, and Conclusion, is expanded with detailed analysis and examples. The aim is to distill lessons from these nationally recognized healthcare organizations to inform broader efforts to align health systems with community needs and achieve performance excellence.
This manuscript is not a primary empirical study using surveys or interviews. Instead, it is a structured qualitative evidence synthesis of publicly available documentary sources describing nationally recognized healthcare organizations over 20 years. The contribution is to consolidate, categorize, and compare documented organizational processes and measurable results associated with community citizenship and performance excellence, producing a practice-relevant cross-case synthesis for health system leaders and scholars. Using a structured qualitative document analysis of award documentation, government reports, and healthcare management literature (2005–2025), this study synthesizes cross-case themes linking performance excellence practices to community citizenship initiatives and reported outcomes.
To address this aim, the study used a structured qualitative document analysis of publicly available sources describing U.S. healthcare organizations recognized for performance excellence between 2005 and 2025. Data were drawn from award documentation, government and quasi-government reports, and healthcare management literature, and then extracted using a standardized abstraction template that captured organizational processes, community citizenship initiatives, and reported performance outcomes. Evidence was analyzed using directed content analysis to code recurring practices and results into thematic domains aligned with performance excellence and healthcare quality management constructs, followed by cross-case synthesis to identify consistent patterns across organizations and time periods [5-7].
Methods
Study Design
This manuscript reports a qualitative evidence synthesis using structured document review and directed content analysis. The purpose was to identify organizational processes and measurable results associated with community citizenship among U.S. healthcare organizations recognized for performance excellence during 2005–2025. The design is best characterized as a qualitative descriptive review with cross-case synthesis, using publicly available documentary evidence as the primary data source. Documentary analysis is an established qualitative method for systematically extracting and interpreting meaning from written materials, particularly when the phenomena of interest are organizational practices, strategies, and reported outcomes embedded in formal documentation [5].
Sampling Frame and Case Identification
The sampling frame consisted of U.S. healthcare organizations that received national recognition for organizational performance excellence in healthcare delivery between 2005 and 2025. “Industry-leading” organizations were operationalized as award recipients and/ or top-tier honorees in publicly documented national performance excellence programs. The 2005–2025 time horizon was selected to capture the longitudinal evolution of performance excellence strategies and the increasing emphasis on community health improvement and the social determinants of health during the value based care era.
Data Sources
Data were collected exclusively from publicly available sources to enable transparency and replicability. To enhance transparency and minimize selection bias, the document identification and screening process was systematically tracked and is summarized in Figure 1 in the Appendix. Consistent with qualitative evidence synthesis guidance, inclusion decisions were based on predefined eligibility criteria and documented at each screening stage to support the auditability of analytic decisions [5,8].
Three categories of documents were included:
1. Award documentation and organizational profiles describing applicant practices, management systems, and results (e.g., award recipient profiles, official summaries).
2. Government and quasi-government reports relevant to quality measurement, safety, performance excellence frameworks, and population health orientation.
3. Peer-reviewed and professional healthcare management literature used to contextualize and triangulate claims found in award documentation and organizational reports.
Using multiple documentary categories strengthens credibility through triangulation, reducing reliance on any single narrative source and improving interpretive robustness in qualitative document-based research [5].
Eligibility Criteria
Documents and organizational cases were included if they met all criteria:
1. The organization was a U.S.-based healthcare delivery organization recognized for performance excellence between 2005 and 2025.
2. Documentation described at least one of the following: organizational strategy deployment, quality and safety management systems, workforce and leadership practices, community engagement programs, or measurable outcomes (clinical, patient experience, workforce, financial, or community health indicators).
3. The document contained sufficient detail to support the extraction of either (a) process elements (what the organization did) or (b) results evidence (what changed, including metrics when available).
Documents were excluded if they were (a) purely promotional marketing materials without process or outcome content, (b) duplicate summaries without additional information, or (c) unrelated to healthcare delivery performance excellence or community citizenship practices.
Data Extraction
A standardized extraction template was used to capture comparable data across organizations and document types. Extracted elements included:
• Organizational characteristics (setting, type of organization when stated)
• Performance excellence approach (strategy deployment, leadership system, management framework references)
• Community citizenship initiatives (community benefit, SDOH initiatives, cross-sector partnerships, workforce pipeline efforts)
• Measurement and results evidence (clinical quality and safety indicators, patient experience, workforce engagement/retention, financial indicators, and community health outcomes when reported)
• Time period of reported outcomes (pre-award, during award cycle, post-award follow-up when available)
To reduce selective emphasis, extraction prioritized (1) explicitly reported metrics, (2) externally benchmarked measures (when described), and (3) repeated measures across years when available. Standardization of extraction is consistent with best practices in qualitative document analysis for supporting systematic comparison across heterogeneous sources [5].
Analytic Strategy
A directed content analysis approach was applied to organize evidence into pre-specified thematic domains derived from performance excellence and healthcare quality management constructs, while allowing inductive subthemes to emerge. Directed content analysis is appropriate when prior theory or established frameworks guide initial coding while still permitting emergent categories to refine the analytic structure [6].
Coding emphasized two analytic targets:
1. Processes, defined as repeatable organizational practices and management routines that plausibly drive performance (e.g., strategy deployment systems, leadership-driven culture work, integrated quality infrastructure, community partnership mechanisms).
2. Results, defined as measurable outcomes reported in the documentary evidence (e.g., infection reductions, patient experience improvements, access metrics, workforce retention, operating margin trends, community screening uptake).
The unit of analysis was the organizational case (a healthcare organization or system), with documents treated as evidence sources for each case. After coding, a cross-case synthesis was conducted to compare patterns across organizations and time periods, with attention to convergence (themes consistently present across cases) and divergence (themes associated with certain organizational types or eras). Cross-case synthesis is widely used in comparative case study methods to identify replicable patterns and plausible mechanisms across settings [7].
Rigor, Credibility, and Transferability
Given that this study uses documentary evidence rather than primary data collection, credibility was strengthened through triangulation across document types (award documentation, government reports, and healthcare management literature). The analytic approach emphasized transparency in how evidence was coded into thematic domains, consistent with established content analysis principles focused on systematic classification and interpretation [8].
Transferability was supported by explicit case inclusion criteria, standardized extraction, and reporting of results as thematic patterns with illustrative metrics rather than generalized causal claims. The analysis is intended to identify plausible, practice-relevant mechanisms and results patterns among recognized high performers, not to estimate effect sizes or establish causal attribution.
Results
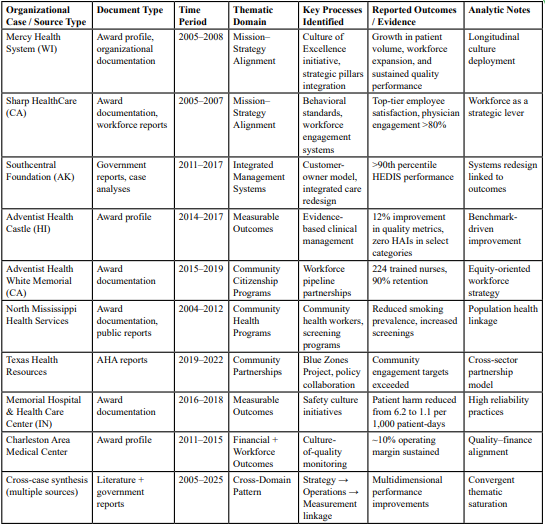
Results reflect the outputs of a structured documentary evidence synthesis rather than primary data collection. Across award documentation, government reports, and healthcare management literature spanning 2005–2025, the analysis identified a consistent set of organizational processes and reported performance outcomes associated with community citizenship among nationally recognized high performers. Directed content analysis yielded three dominant thematic domains, and cross-case synthesis demonstrated convergence in how organizations align mission and strategy, deploy community programs, and report multidimensional performance results. The sections that follow summarize the evidence base, present the thematic domains with illustrative examples, and describe cross-case patterns and limitations of the documentary record. Table 1 summarizes the documentary evidence base, linking organizational cases, document types, thematic domains, and extracted qualitative findings. The table enhances transparency by demonstrating how multiple documentary sources and organizational contexts supported thematic domains, consistent with best practices in structured qualitative document analysis [5].
Overview of the Evidence Base
The structured review yielded a multi-source documentary dataset describing performance excellence practices and community citizenship initiatives among nationally recognized healthcare organizations between 2005 and 2025. Evidence included award documentation describing organizational systems and strategy deployment, public reports and summaries referencing performance benchmarks, and healthcare management literature used for contextual triangulation.
Thematic Domains Identified Through Directed Content Analysis
Across cases, evidence clustered into three major domains that explain how high-performing organizations operationalized “community citizenship” while sustaining excellence in quality and organizational performance.
Domain 1, Mission-Strategy Alignment and Integrated Management Systems
Organizations consistently described mission-driven strategic planning linked to measurable objectives, frequently operationalized through integrated management frameworks. Evidence emphasized leadership system alignment, workforce engagement as a strategic lever, and deployment of organizational standards and routines that translated mission into daily practice. This domain also included explicit use of measurement systems and benchmarking targets, such as aiming for top-decile performance and tracking progress longitudinally.
Domain 2, Community Citizenship as a Portfolio of Programs and Partnerships
Community citizenship was operationalized through a portfolio approach that included community benefit investments, culturally aligned workforce pipeline programs, cross-sector partnerships, and targeted initiatives addressing social determinants of health. Programs were typically presented as strategic extensions of the organization’s mission rather than peripheral community relations activities. In many cases, community-facing initiatives were linked to measurable participation outputs and, when available, community level outcomes.
Domain 3, Measurable Performance Outcomes Across Multiple Stakeholder Dimensions
Award documentation and related reports frequently included measurable results spanning clinical quality and safety, patient experience, workforce engagement and retention, access and care coordination, and financial stewardship. The documentary evidence supports a pattern of multidimensional performance, in which organizations reported improvements across several outcome categories simultaneously, suggesting the presence of reinforcing operational capabilities rather than isolated interventions.
Cross-Case Pattern: Process-to-Results Consistency
Across organizations and over the two-decade time horizon, the analysis identified a consistent “process-to-results” narrative structure in the evidence base: leadership and strategy deployment systems were linked to operational improvement routines, which in turn were linked to measurable outcomes and community-facing investments. While the specific initiatives varied by local context, the recurring mechanism was a systematic management approach combined with explicit measurement and continuous improvement.
Nature of Results, Evidence, and Data Limitations
The evidence base contained a mix of quantitative and qualitative results statements. Quantitative metrics were more consistently reported for clinical outcomes and patient experience than for community-level population health outcomes, which were sometimes described narratively rather than using standardized measures. As a result, findings are best interpreted as transferable patterns of high-performance practice supported by illustrative metrics, rather than a comprehensive comparative effectiveness evaluation across all organizations.
Mission and Strategy
A unifying theme among top-performing healthcare organizations is a mission-driven strategy centered on excellence and community service. These hospitals and health systems commonly establish a culture of excellence as a strategic foundation for achieving their mission. For example, Mercy Health System in Wisconsin, a 2007 award recipient, spent nearly two decades cultivating what it termed a “Culture of Excellence” initiative to drive quality and service [3]. This long-term commitment was embedded into Mercy’s strategic pillars (quality, service, partnering, and finance), ensuring that daily operations and leadership decisions aligned with the mission of delivering outstanding patient care and community benefit. Mercy’s strategy exemplified how visionary leadership and sustained focus can transform an organization. Since 1989, Mercy has seen tenfold growth in patient visits and dramatic increases in revenue and staffing, while maintaining high-quality standards [9].
Sharp HealthCare in San Diego, honored in 2007, built its strategy around “The Sharp Experience,” a mission to make Sharp the best place to work, practice medicine, and receive care. Leadership at Sharp engaged over 1,000 employees in developing behavioral standards and process improvements to reinforce this mission [10]. The result was a delighted workforce and physician network— Sharp’s employee satisfaction ranked “best in class” nationally, and over 80% of its physicians rated Sharp as the best place to practice medicine [10]. These human-capital outcomes were no accident; Sharp’s strategy invested heavily in staff development, including a corporate university and annual education stipends, to build internal capacity for excellence. In turn, a motivated, skilled workforce drove innovations in patient-centered care and efficiency, illustrating the strategic payoff of aligning mission, people, and performance goals.
Another hallmark is strategic planning with a systems perspective. Many honorees adopted the national performance-excellence framework as a blueprint for strategy execution, which evaluates seven key areas from leadership and strategy to customers, workforce, operations, and results providing an integrated management system [1]. Southcentral Foundation in Alaska, a two-time honoree (2011, 2017), used this systems approach to redesign its entire health system around customer needs. SCF’s mission as an Alaska Native-owned system is to achieve physical, mental, social, and spiritual wellness for its community. To fulfill this, SCF leaders engaged tribal stakeholders to develop a clear vision and operating model for integrated care. They broke down silos between primary care, behavioral health, and specialty services, and even co-designed facility layouts with cultural input [11]. The strategic intent was ownership patients (called “customer-owners”) feel ownership of their health system and share responsibility for outcomes. SCF’s model demonstrates how mission and strategy centered on community ownership can yield an innovative care system that is adaptable and resilient [11].
Finally, these organizations embed measurable goals into their strategy. Top performers set ambitious targets (often “top decile” or better on national benchmarks) for clinical quality, patient satisfaction, and efficiency and use data extensively to guide decisions. For example, Adventist Health Castle in Hawai‘i, a 2017 award recipient, aimed to rank in the top 25% of hospitals nationwide on composite patient safety and clinical quality measures and succeeded by improving those metrics by 12% over three years [12]. Castle’s strategic focus on evidence-based practices led to zero hospital-acquired infections in several categories and top-tier mortality outcomes [12]. Similarly, Charleston Area Medical Center in West Virginia set a vision of “best care” and monitored its progress via an annual employee survey on patient focus; by 2015, it ranked in the top 10% nationally on this culture-of-quality index [13]. In sum, award-winning providers marry an inspiring mission (“world-class care for our community”) with systematic strategy deployment and rigorous goal-setting. This alignment has proven effective across large academic systems and small rural hospitals alike, yielding role-model organizations in U.S. healthcare.
Community Programs
Excellence in healthcare extends beyond hospital walls a fact well understood by these nationally recognized organizations. A distinguishing characteristic of award recipients is their deep engagement in community health programs and partnerships that address public health needs, health equity, and the social determinants of health. Over 20 years, winners consistently demonstrated a “passion and continuous commitment to making communities healthier and more vital,” often earning separate accolades for community service, such as the Foster G. McGaw Prize [14].
One approach is a significant investment in community benefit activities. Sharp HealthCare, for example, quantified the economic value of its community services including charity care, health education, free screenings, and staff volunteerism and grew that investment from $100 million in 2001 to over $180 million by 2006. During that same time, Sharp’s direct support for vulnerable populations (e.g., covering undercompensated care and health research for the underserved) increased from $4 million to $6.5 million. This expansion of community programs was not by chance; Sharp leadership deliberately targeted community health needs in its strategic planning, collaborating with public officials whenever new health threats were identified to implement “safe, evidence-based, and equitable solutions” [12]. Moreover, Sharp encouraged its management and staff to engage personally with the community. The hours that Sharp managers volunteered for community programs increased from 10,000 in 2003 to almost 60,000 in 2006. These efforts fostered trust and partnership with the community, illustrating how an organization’s community-oriented mission translates into on-the-ground impact [10].
Many honorees also launch programs targeting specific local needs, often in collaboration with other sectors. Health professional training and education are notable examples. Adventist Health White Memorial in Los Angeles, a 2019 award recipient serving a predominantly Hispanic community, recognized the need for a culturally representative healthcare workforce. In response, White Memorial partnered with local schools and foundations to train more than 224 residents in nursing over the course of two decades. Impressively, 100% of these trainees achieved Registered Nurse licensure, and 90% remained employed at White Memorial after three years building a nursing staff that “reflects the demographics of [the] community” and can provide culturally competent care in patients’ primary language [15]. This program simultaneously addresses community economic development, diversity, and hospital staffing, and it exemplifies how community engagement and equity can be advanced together through strategic workforce initiatives.
Award-winning systems often address broader public health challenges through multi-pronged programs. Preventive health and wellness initiatives are common, such as Texas Health Resources’ Blue Zones Project in Fort Worth. Texas Health, which earned the 2022 McGaw Prize, led a neighborhood-by-neighborhood initiative encouraging healthy lifestyle changes from diet and exercise to tobacco cessation and helped implement citywide policies to promote health. The project exceeded its targets for resident engagement and became a model cited for significantly improving the community’s health status [14]. In rural Maine, Franklin Memorial Hospital (a 2005 finalist) spearheaded a Healthy Community Coalition to bring mobile health screenings and education to isolated areas [16]. In the Mississippi Delta, North Mississippi Health Services, a 2012 honoree, deployed community health workers to increase diabetes management and cancer screening rates [17]. These programs demonstrate innovation in care delivery beyond clinical walls meeting people where they live, work, and play.
Several recipients have also tackled the social determinants of health through partnerships. Memorial Hermann Health System in Texas and UMass Memorial Medical Center in Massachusetts both recognized for community excellence addressed food insecurity with “Food as Medicine” programs and expanded access to healthy foods in food deserts [14]. Others, such as MUSC Health in South Carolina, influenced public policy to benefit community health; MUSC worked with legislators to improve rural broadband and telehealth access, thereby reaching underserved rural patients and advancing health equity statewide [14].
Critically, during crises, these organizations step up as community anchors. In the COVID-19 pandemic, many prior awardees leveraged their community trust and infrastructure to respond swiftly. Texas Health Resources, for instance, prioritized vaccinating at-risk community members by deploying mobile health units and culturally appropriate outreach in minority neighborhoods. It served as “an example for how to redeploy resources… and support community members during a public health emergency” [14]. Likewise, UMass Memorial coordinated closely with local public health departments on vaccine rollout and even had senior leaders go “feet on the street” in low-income areas to build vaccine confidence [14]. Such actions underscore the point that performance-excellence hospitals view community health improvement as core to their mission not a peripheral activity. By forming strong community partnerships, regularly assessing local needs through Community Health Needs Assessments, and innovating solutions, these organizations translate their commitment to community benefit into tangible health outcomes [2].
Measurable Impacts
The ultimate hallmark of these nationally recognized organizations is their track record of superior results. Across clinical quality, patient outcomes, patient experience, workforce metrics, and financial stewardship, award-winning healthcare organizations significantly outperform their peers, often sustaining top-tier performance over many years. A 2011 Thomson Reuters study found that hospitals recognized for performance excellence or even those reaching the finalist stage were six times more likely to be among the nation’s “100 Top Hospitals” and consistently outperformed average hospitals on key care measures [1]. This section highlights measurable impacts achieved by such organizations over the past 20 years, demonstrating that a focus on excellence yields real-world benefits for patients and communities.
Clinical Quality and Patient Safety. Many honorees have achieved clinical outcomes in the top 10% nationally for major quality indicators. For example, St. David’s HealthCare in Austin, Texas, met or exceeded top-decile performance on all Centers for Medicare & Medicaid Services (CMS) core quality measures for four consecutive years leading up to its award. It also drove patient satisfaction upward each year through a “Service Excellence” initiative, coinciding with high adherence to evidence-based care [18]. Other winners virtually eliminated specific harms: Memorial Hospital and Health Care Center in Jasper, Indiana, reported zero early-elective deliveries, zero pressure ulcers, and zero MRSA infections in the years prior to its 2018 award [19]. Similarly, Adventist Health Castle in Hawai‘i maintained zero catheter-associated UTIs for more than 3 years and zero ICU central-line infections in 4 of 5 years placing it in the elite tier nationwide for patient safety outcomes [12]. These results illustrate a broader trend: award-winning hospitals often have infection, mortality, and complication rates significantly better than national averages, reflecting highly reliable care processes. For instance, Con a composite patient safety index, Memorial Hospital’s performance ranked in the top 10% of all hospitals, with total patient harm events reduced from 6.2 to 1.1 per 1,000 patient-days in just two years [19].
Access and Care Innovation. Top-performing systems also improved access to care and care coordination, often with a measurable impact on population health. Southcentral Foundation provides a compelling example. By adopting “optimized access” principles, SCF ensured that 70% of behavioral health patients received same-day consultations, integrating mental health into primary care to reduce wait times for a vulnerable population [11]. This immediate-access behavioral health model is well above typical benchmarks and has contributed to better continuity of care. SCF’s overall performance has exceeded the 90th percentile on HEDIS measures (standard preventive and chronic care metrics) in its service area [11]. Other systems show improvements in community health outcomes: North Mississippi Health Services increased colorectal cancer screening rates and helped drive down the adult smoking rate in its region by seven percentage points (to 15.6%) between 2004 and 2012 [17]. These outcomes align with NMHS’s targeted community wellness programs and chronic disease management efforts, demonstrating that aligning with public health goals, such as tobacco cessation, can yield measurable regional health gains.
Patient Experience and Satisfaction. Virtually all award recipients rigorously measure patient experience, and many achieve top-quartile satisfaction. For seven consecutive years, Kindred Nursing Center– Mountain Valley, a 2016 honoree in long-term care, received a 100% satisfaction rate from its residents and families far above industry norms [2]. In acute care, several hospitals achieved 90th-percentile patient recommendation scores. Memorial Hermann Sugar Land Hospital, for instance, saw its patients’ likelihood-to-recommend scores reach the Press Ganey 90th percentile across multiple service lines [2]. High patient satisfaction often went hand in hand with high clinical quality. Hill Country Memorial in Fredericksburg, Texas, ranked in the top 10% nationally for both patient satisfaction and outcomes in surgery, safety, and joint replacement, according to independent ratings [18]. This alignment suggests that organizations can excel at the patient-centered aspects of care while delivering excellent clinical outcomes a dual achievement that marks comprehensive performance excellence.
Workforce and Financial Outcomes. Internally, these organizations nurture environments that support staff and financial sustainability, which, in turn, reinforce excellence in patient care. Many honorees significantly outperform benchmarks in staff engagement and retention. Kindred’s 90% employee retention rate was 20% higher than the national average for nursing facilities [2]. Memorial Hermann Sugar Land similarly retained more than 90% of its employees and 100% of its physician partners in 2016 an enviable retention rate signaling a strong workplace culture [2]. High workforce stability contributes to better care continuity and institutional knowledge. Additionally, physician engagement scores at top institutions are often exemplary. For example, Adventist Health Castle’s physicians ranked the hospital in the top 10% nationally for practice environment and for its commitment to safety and quality [12].
Financial stewardship also underpins these organizations’ success. Many winners maintained healthy margins and continued to grow while expanding community services. Charleston Area Medical Center Health System, for example, sustained an operating margin near 10% every year from 2011 onward, despite providing above-average levels of uncompensated care in a poor region [13]. Its financial strength exceeded benchmarks for comparable teaching hospitals, proving that a safety-net health system can remain financially viable through efficiency and strategic management. Hill Country Memorial nearly doubled its net income (from $10 million to $19 million) in the three years prior to its award, while simultaneously improving its debt-to-cash ratios and earning national recognition for quality and community hospital excellence [18]. These data dispel the notion that focusing on quality is at odds with financial performance. In fact, the two often go hand in hand. As summarized by the U.S. Commerce Secretary, the cumulative impact of the national performance excellence program is estimated at $1 billion per year in economic benefits due to cost savings and efficiency gains among award-winning organizations [20].
In summary, measurable impacts from the past 20 years of excellence award recipients include significantly lower patient harm events, top-tier process-of-care measures, improved population health metrics, superior patient satisfaction, high workforce retention and engagement, and strong financial outcomes. External benchmarks validate these achievements and, in many cases, sustained over time. They demonstrate that pursuing a path of performance excellence yields real benefits for patients and communities. Moreover, the consistency of these results across settings from small rural hospitals to large urban systems indicates that the core concepts of mission-driven leadership, systematic quality management, and community focus are broadly applicable and effective.
Discussion
The patterns observed across two decades of honorees reveal several key practices and principles that drive exceptional performance in healthcare organizations.
Leadership and culture are paramount. Almost every award-winning hospital system was guided by visionary leaders who established a clear mission and fostered a culture of continuous improvement. These leaders did more than set goals they actively engaged staff at all levels in the quality journey, creating buy-in and accountability for excellence [3]. For example, CEOs like Javon Bea of Mercy Health System and Katherine Gottlieb of Southcentral Foundation are often cited for championing quality initiatives, such as Mercy’s physician partnership model and SCF’s Nuka redesign, that fundamentally changed their organizations [11]. Leadership continuity and commitment help explain why many of these organizations sustained high performance even amid industry changes. It is also notable that several health systems, including Henry Ford Health System and Southcentral Foundation, received recognition more than once, suggesting that embedding excellence into culture yields lasting benefits that can be revisited and enhanced over time [12].
A holistic, systematic management framework underpins success. The award criteria function as a comprehensive blueprint covering strategic planning, customer focus, measurement, workforce, and operations [1]. The broad adoption of this framework in healthcare has been documented; since the healthcare category was added in 1999, more than half of all award applicants have come from healthcare [2]. By using such a framework, hospitals ensure they are not excelling in just one department or outcome, but instead improving organization-wide. This systems perspective was evident in cases such as Tennessee hospital networks that applied the framework to drive culture change and performance gains [21]. The comprehensive self-assessment and feedback processes associated with the awards also contribute to ongoing learning. In fact, even applicants who did not win often improved substantially by incorporating feedback [1]. Thus, the disciplined use of an excellence framework and data-driven management is a distinguishing factor separating these organizations from average performers.
Focusing on community health and equity provides a strategic advantage. The past 20 years have seen healthcare move toward population health management and the addressing of social determinants, and award-winning organizations were often ahead of this curve. They forged strong community partnerships, which in turn bolstered their reputation, trust, and market share [16]. For instance, Memorial Hospital in Indiana held more than 70% inpatient market share in its county prior to its award, in part due to its reputation as the preferred community caregiver and employer [19]. Emphasis on health equity, such as diversifying the workforce at White Memorial or improving rural access via telehealth at MUSC Health, positioned these organizations as leaders in addressing disparities [4,14]. During the COVID-19 pandemic, such community trust and outreach capacity translated into effective public health responses, reinforcing the value proposition of hospitals as community anchors [14]. By aligning institutional success with community well-being, these organizations created a virtuous cycle: healthier communities yield lower costs and better outcomes, which benefit hospital performance metrics under value-based care models.
Innovation and adaptability emerged as critical traits. Many of these award-winning providers were early adopters of healthcare innovations, whether in care delivery (integrating behavioral health, patient-centered medical homes, Lean process improvements) or in technology (electronic health records, telemedicine, data analytics). For example, WellStar Paulding Hospital in Georgia, a 2020 recipient, opened as a “greenfield” facility with all private rooms and advanced infection control design, leveraging real-time location systems to improve throughput [22]. Henry Ford Health System, recognized in 2011, pioneered the “No Harm Campaign” that significantly reduced medical errors system-wide, an innovation later informing national safety projects. What set these organizations apart was not just innovating, but scaling and sustaining innovations. They measured outcomes and refined approaches until improvements were sustained, as in Sutter Davis Hospital’s redesign of emergency department processes that halved wait times. Adaptability was also seen in how organizations responded to external challenges: several winners navigated recessions or healthcare reform by remaining agile diversifying services, pursuing partnerships, and continuing to invest in quality [1]. This resilience has been quantified: one national analysis estimated a 820:1 return on investment in the performance-excellence program, accounting for cost savings and societal benefits from improvements among applicants [21].
In reflection, it is clear that while technology and medical practice have evolved since 2005, the core drivers of excellence in healthcare remain consistent. Patient-centered mission, engaged workforce, rigorous processes, community partnership, and continual learning define the leading organizations across the era. These factors are interdependent: without a supportive culture, adopting new technology will not yield better outcomes; without community trust, cutting-edge clinical services may not reach those in need. High-performing organizations orchestrate all these elements in concert, which is precisely what the national award criteria encourage.
Conclusion
In two decades of national performance-excellence awards in healthcare, U.S. hospitals and health systems have demonstrated that transformative improvements in quality and community health are both achievable and sustainable. From the mid-2000s through the mid-2020s, a diverse array of organizations including academic medical centers, integrated delivery networks, community hospitals, rural clinics, and long-term care facilities earned recognition by achieving world-class outcomes while staying true to their missions [2,15].
A key takeaway is that excellence is a journey, not a destination. Many of the profiled organizations embarked on multi-year (even multi-decade) journeys of cultural change and process redesign. They did not view the award as an endpoint, but rather as confirmation they were on the right path a path they continue to follow beyond recognition [3,11]. The practices that matter strategic focus on patients and quality, empowerment of employees and physicians, data-driven decision-making, and deep commitment to community well-being can be adopted by any healthcare organization, regardless of size or geography.
The equally weighted span of examples from 2005 through 2025 also demonstrates that performance excellence is timeless. Early pioneers like Sharp HealthCare and Mercy Health System set benchmarks that remain relevant today, while more recent innovators such as Adventist Health White Memorial and Texas Health Resources continue to advance community health and equity [10,14,15]. As healthcare faces new pressures from pandemics to workforce shortages to persistent inequities the stories of these organizations serve as evidence and inspiration that excellence is possible even in turbulent environments. Future hospitals can look to these role-model peers as “north stars” on the journey to delivering safer, more competent, and more community-centered care for all.
Competing interests:
The authors declare that they have no competing interests.
References
Thomson Reuters. (2011). Baldrige award recipient study: Impact of performance excellence in healthcare. Baldrige Foundation.
National Institute of Standards and Technology. (2016). Results with Baldrige in health care. NIST. View
Quality Digest. (2008, January 10). 2007 Malcolm Baldrige National Quality Award winner: Mercy Health System. View
National Institute of Standards and Technology. (2019). Adventist Health White Memorial: Award recipient profile. NIST. View
Bowen, Glenn A. (2009). “Document Analysis as a Qualitative Research Method.” Qualitative Research Journal, 9 (2): 27–40. View
Hsieh, Hsiu-Fang, and Sarah E. Shannon. (2005). “Three Approaches to Qualitative Content Analysis.” Qualitative Health Research, 15 (9): 1277–88. View
Yin, Robert K. (2018). Case Study Research and Applications: Design and Methods. 6th ed. Thousand Oaks, CA: SAGE. View
Krippendorff, Klaus. (2018). Content Analysis: An Introduction to Its Methodology. 4th ed. Thousand Oaks, CA: SAGE. View
Reliable Plant. (2008, April 23). Five organizations receive the Baldrige Quality Award. ReliablePlant.com. View
National Institute of Standards and Technology. (2007). Sharp HealthCare: Award recipient profile. NIST. View
Collins, B., & Berwick, D. (2015). Intentional whole health system redesign: Southcentral Foundation’s “Nuka” system of care. The King’s Fund. View
National Institute of Standards and Technology. (2017). Adventist Health Castle: Award recipient profile. NIST. View
National Institute of Standards and Technology. (2015). Charleston Area Medical Center Health System: Award recipient profile. NIST. View
American Hospital Association. (2022, April 19). Texas Health Resources awarded the 2022 Foster G. McGaw Prize for excellence in community service [Press release]. AHA News. View
National Institute of Standards and Technology. (2019, November 14). Six health care, nonprofit, and education organizations win national awards for performance excellence [Press release]. NIST. View
Klein, S. (2014). Profile: Heartland Regional Medical Center ACO. The Commonwealth Fund. View
National Institute of Standards and Technology. (2012). North Mississippi Health Services: Award recipient profile. NIST. View
National Institute of Standards and Technology. (2014). Four U.S. organizations honored with 2014 national quality award [Press release]. NIST. View
National Institute of Standards and Technology. (2018). Memorial Hospital and Health Care Center: Award recipient profile. NIST. View
U.S. Department of Commerce, National Institute of Standards and Technology. (2014). Four U.S. organizations honored with 2014 national quality award [Press release]. NIST. View
American College of Healthcare Executives. (2025). Baldrige Program – Using the Baldrige Leadership Model to overcome evasive organizational challenges. ACHE. View
National Institute of Standards and Technology. (n.d.). Results with Baldrige in health care. NIST. View