Journal of Mental Health and Social Behaviour Volume 2 (2020), Article ID: JMHSB-116
https://doi.org/10.33790/jmhsb1100116Mini Review
Determinants of Risky Sexual Behaviors in an HBCU Community
Emory L. Perkins, LCSW, ACSW, LMFT*, Fabio Chacon, Cordelia Obizoba, RN, Brade-Stennis, K, Rita Wutoh, Leroy Madison, Gregory Wells, Denote' Turner
Department of Social Work, Bowie State University, 1400 Jericho Park Road, Bowie, MD, 20715, 30863127, United States
Corresponding Author Details: Dr. Emory L. Perkins, LCSW, ACSW, LMFT, Assistant Professor, Department of Social Work, Bowie State University, 1400 Jericho Park Road, Bowie, MD, 20715, United States. E-mail: Eperkins@bowiestate.edu
Received date: 28th March, 2020
Accepted date: 28th April, 2020
Published date: 30th April, 2020
Citation: Perkins, E.L., Chacon, F., Obizoba, C., Stennis, K.B., & Wutoh, R. (2020). Determinants of Risky Sexual Behaviors in an HBCU Community. J Ment Health Soc Behav 2(2):116.
Copyright: ©2020, This is an open-access article distributed under the terms of the Creative Commons Attribution License 4.0, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited. Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original author and source are credited
Abstract
After four decades of HIV/AIDS pandemic, African Americans represent at least 43 percent of infections but only makeup 12.6 percent of the USA population (Census Bureau, 2010). It is apparent from these rates that additional information is needed to further understand the possible linkages between HIV/AIDS infection and members of this ethnic group. This exploratory study analyzed relationships between knowledge and attitudes toward safe sex, and risky behaviors on an HBCU. Using purposive sampling, a group of 364 students was surveyed. Factors assessed as determinants of risky sexual behaviors were: (1) general HIV knowledge, (2) attitude towards safe sex practices, and (3) unprotected or unsafe sex practices. Findings suggest that the average count of risk incidents among women was significantly higher than men; however, women are more inclined to have preventive contagion practices for sexually transmitted diseases than men. In addition, they are more aware of what constitutes risky sexual behavior. The findings should assist universities in developing educational programs and culturally sensitive intervention and prevention strategies aimed at students who are at risk for participating in risky behaviors.
Keywords
HIV/AIDS, knowledge, attitudes, risky sexual behaviors
Introduction
The young adult years (ages 18-24) are fraught with decision making, including those related to college attendance and sexual behavior. Many who decide to enter college also decide to engage in risky sexual behaviors perhaps as a component of discerning their identity versus role confusion, as purported by Erickson in his Stages of Development Theory. Perera and Abeysena [1] noted that the young age of the majority of the undergraduate students predisposes them to risky sexual behaviors, henceforth referred to as RSBs. Similarly, Yi, et al. [2] found that University undergraduate students have social and behavioral characteristics that are associated with RSBs. The social context of university lifestyle in addition to individual, cultural differences, and structural factors were perceived to affect risky sex through high levels of alcohol consumption, increased sexual opportunities, liberation from moral surveillance and expectations of the stereotypical highly sexually active student Chanakira, et al. [3]. Health risky behaviors of unprotected sex, multiple and concurrent sex partners, drugs including risky smoking and alcohol resulting in sexually transmitted infections (STIs) has been reported in several studies [1,4,6].
Although in its fourth decade, there are still implications for public health care and safe sex education regarding Human Immunodeficiency Virus (HIV), Acquired Immune Deficiency Syndrome Immune Deficiency (AIDS) and other STIs, STDs and unplanned pregnancy, particularly with those who indulge in RSBs like students in college. Burnett, et al. [7] noted that HIV, AIDS, STIs, and unwanted pregnancy continue to impact young adults in the United States at a disproportionate rate, particularly during the college years. The presence of some STIs greatly increases the likelihood of acquiring or transmitting HIV (Centers for Disease Control and Prevention [8]. Haile et al. [4] noted that HIV risk perception has been low despite the high prevalence of RSBs among college students. Similarly, Murray et al. [9] concluded that misperceptions about HIV have implications for unintended sexual transmission of HIV.
According to the CDC HIV Surveillance Report [15], Blacks/African Americans account for a higher proportion of new HIV diagnoses and people living with HIV, compared to other races/ethnicities. Among men and women, CDC stated that generally, receptive sex is riskier than insertive sex hence women have a higher risk of getting HIV during vaginal or anal sex than their sex partners. Supporting the Black/African American women HIV statistics, Pittman et al. [6] noted that Black adult women ages 18-25 years are among the fastest-growing demographics of HIV infection, second only to men who have sex with men. Prior studies have examined the effects of HIV/AIDS knowledge and attitude on undergraduate students RSBs, however only a few of the studies focused specifically on gender attributes of RSBs and STIs/HIV.
In addition to Black women being disproportionately affected by HIV, limited research has examined race and gender as moderator variables of RSBs and HIV influences [16]. In a study on comparison of HIV Knowledge, Attitudes, and Sources of STI Information between female and male college students in Taiwan, Tung et al. [17] found that while male and female students reported moderate knowledge and attitudes, females had more positive attitudes toward people with HIV/AIDS than males. Contrarily, Sabato [18] noted evidence of varying degrees of knowledge, with greater awareness among females than males, sexual risks for HIV transmission more prominent among males, but without a cause and effect relationship between knowledge of HIV and risk behaviors. In contrast to Sabato [18] findings of no cause and effect relationship, Wang et al. [19] found positive associations between RSB and HIV knowledge.
Burnett et al. [7], surveyed a sample of 1,874 university students aged 16-54 years to determine if sexually active males versus females with external, unstable, and specific causal attribution (i.e., external locus of control) engaged in safer sexual practices (e.g., condom use) and lesser alcohol and legal/illicit drug use. The study revealed that male students with an external attributional style engaged in a greater number of unsafe sexual behaviors (e.g., multiple partners) and higher amounts of alcohol and drug use than female students. Additionally, for both males and females, an internal attributional style was associated with greater drug use and a greater likelihood to engage in HIV-related risk behavior.
In a study on sexual victimization and benefit expectations of risky behavior among female college students, Carlson and Duckworth [20] noted that sexual victimization has been shown to positively relate to both engagements in risky behavior and subsequent sexual victimization. Scull et al. [21] affirmed that higher intentions to engage in RSBs were associated with gender and sexual experience, but also with having lower intentions to communicate with a sexual partner about pregnancy and STIs, and having higher gender norm endorsement. Similarly, on gender factors, Burns [22] concluded that while male students and hazardous drinkers were most likely to participate in unprotected sex and regretted sex, female students and hazardous drinkers were most likely to experience an unwanted sexual advance. Attention has to be given on the role of alcohol and/ or drug abuse in the participation of HIV risk behaviors in the design and implementation of HIV prevention for university students [23].
This quantitative exploratory study is significantly important as the university student population is particularly involved in health risk behaviors. Research has focused on the degree to which women consider the risks or costs of engaging in risky behaviors[20]. Understanding the factors associated with RSBs is a necessary step to effective interventions concluded that campus-based student peer educators may be effective in educating freshman students about HIV and RSBs. Preventing RSBs among undergraduate African American students through knowledge of and positive attitude towards HIV/ AIDS would contribute to the prevention of unwanted pregnancies as well as HIV and other STIs[2]. Using the Social Cognitive Theory, which posits that knowledge of health risks creates the precondition for behavior change [9], the primary aim of this study was to assess gender differences in HIV knowledge and attitudes in relation to RSBs. As females are noted to have more HIV risks than males and with more female students in HBCUs, research data on male and female perspectives of RSBs can inform university administration health promotion services on reducing the prevalence of STIs/HIV among young adults.
Method
Research Design
Investigators tested four research hypotheses using an ex-post facto, quasi-experimental research design. This afforded the opportunity to test the relationship between attitudes and healthier sexual practices and knowledge of HIV and risk-taking behaviors. It allowed the researchers to discern which groups tended to engage in risk-taking behaviors with respect to sexual practices. There was no opportunity to manipulate knowledge of HIV/AIDS or sexual practices and risk-taking behaviors, as these variables were assessed after the initial study.
Sampling Procedures
The participants included a sample of 364 college students ranging from 18 to 39 years of age. The study was granted IRB by the institution. A convenience (non-probabilistic) sample of 10-course sections at the undergraduate level was surveyed. Participation was voluntary and anonymous, under informed consent. Exclusion criteria included: 1) age less than 18 years old, 2) age greater than 39 and 3) ethnicity other than African American. Inclusion criteria included that participants must be currently enrolled as a student.
Data Collection Procedures
Data were obtained through two self-assessment tools completed by each participant; The first instrument – KAB Scale - is adapted from the CDC College Health and Risk Behavior Survey, which assesses sexual practices and condom usage. The second instrument is an HIV Knowledge Questionnaire (HIV-KQ-45), authored by Carey et al. [24]. The researchers trained and oriented undergraduate students on how to conduct and administer the research instruments as paper and pencil surveys. Four professors granted permission to the researcher to survey students in their upper-level undergraduate courses and in sections of the Freshman Seminar course. The participants received information that their participation was voluntary and confidential. Incentives for participation included enrollment in a raffle for an iPod and two $50 prizes. Only participants who met the eligibility criteria were allowed to participate in the study. The privacy of names was preserved by the researchers both in the assignment and coding of questionnaires.
Perpetuates & Protective Factors
The KAB Behavior Scale consists of a 77-item questionnaire that assessed five areas of behavior: 1) general HIV/AIDS knowledge questions; 2) culturally based questions that included conspiracy theories and, perceived vulnerability and severity of HIV/AIDS; 3) attitudes about condom use and sex; 4) self-efficacy questions; and 5) information about sexual behaviors, practices, and beliefs. The second instrument is the HIV Knowledge Questionnaire (HIVKQ- 45), which assessed the participant’s knowledge about HIV/ AIDS.
Additionally, each participant was given the demographic questionnaires to record their responses. Ten items are included: age, gender, race, ethnicity, classification, residence status, employment status, student status, number of children, and highest level your mother/female guardian completed in school.
Data Analysis
The analysis for this investigation was quantitative. A t-test, chisquare, one-way ANOVA and Pearson correlations were used to analyze the data with the IBM-Statistical Package for the Social Sciences SPSS. The analysis occurred in two stages:
1-The stage one focused on descriptive analysis of the sample in the form of tables of frequencies, percentages and means. These data allowed the researcher to glean contrasting and converging patterns in variables within, across and among groups.
2-The stage two focused on five research hypotheses; Sig.= 0.01 was set for all hypotheses testing.
Results
Demographic Profile of the Participants
An analysis of the demographics analysis provides information about variables that may impact the results such as gender, age, education, employment status, income, sexual orientation, number of children and residency.
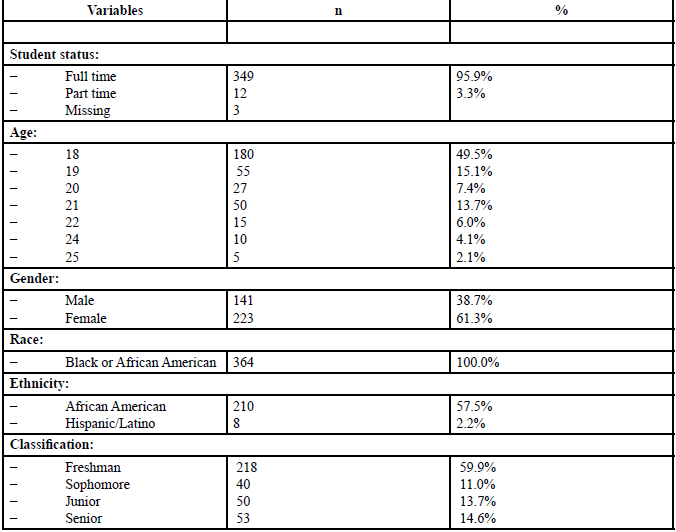
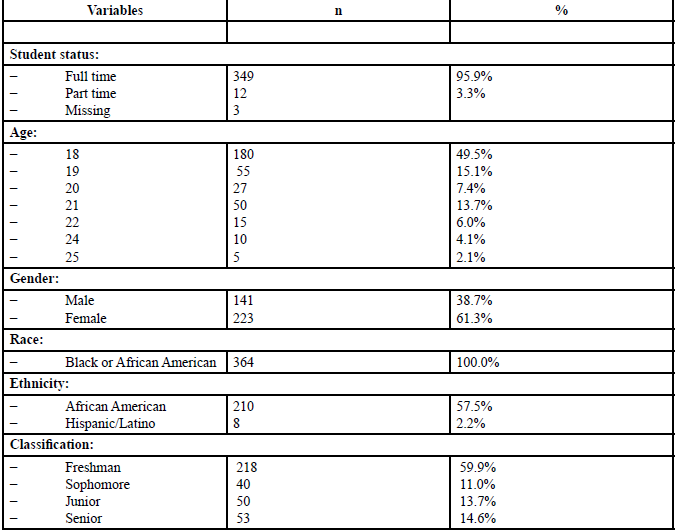
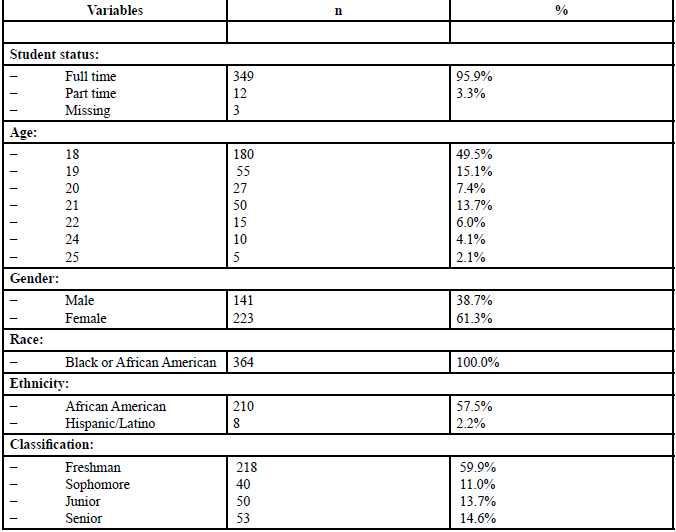
As displayed in Table 1, the sample (N = 364) consisted of students of both sexes aged 17 to 39 with a mean age of 24. The student status consisted of 349 full-time students (93 %) and 12 part-time students (3.9%). There were 180 students, aged 18, 55 students aged 19, 27 students aged 20, 50 students, aged 22, 10 students, aged 24 and 5 students aged 25. Most participants were female (61.1%) and 38.7 % were male. The majority of the participants self-identified as African-Americans and only 2.2% as Hispanic/Latino. In terms of the students’ classification, 59.9% of the participants were freshmen, 11% of the participants were sophomores, 33.7% of the participants were juniors and 14.6% of the participants were seniors. The aforementioned samples was representative of the university’s larger population.
Discussion
Summary of Findings
This study tested five research hypotheses utilizing independent t-test, chi-square, Pearson correlation, and bivariate correlation or one-way ANOVA..
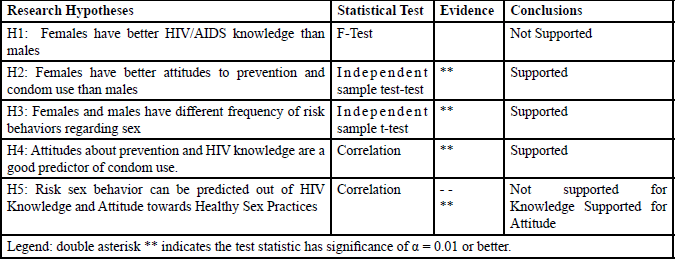
H1: Females have better HIV/AIDS knowledge than males.
H2: Females have better attitudes to prevention and condom use than males.
H3: Males and females differ in their frequency of risk behaviors regarding sex.
H4: Attitudes about prevention and HIV knowledge is a good prediction of condom use.
H5: Risky sex behavior can be predicted out of HIV Knowledge and Attitude towards Healthy Sex Practices.
Findings show the average count of risk incidents among women (116) was significantly higher than men (77). However, using an independent samples t-test, another finding supports that women have better safe sex attitudes compared to men. Females also had a higher knowledge score than males. Also, females are more inclined to have preventive HIV-contagion practices than males, and they are more aware of what constitutes risky sexual behavior. More than half of the respondents reported no condom use. The older, upperclassmen used condoms less. Although almost all the respondents were aware that HIV testing is available on campus, about 41% have never been tested.
As displayed in Table 3, the count HIV risk incidences between females and males, where a chi-square was used to measure gender. Sexual risk incidents for males were 71, while the sexual riskincidents for females were 116. The total sexual risk incidents for all of the respondents were 193. The proportion of male respondents was 40% and the proportion for females was 60%.
As displayed in Table 4, the academic level of the respondents versus knowledge of HIV, respondents showed that there is no significant difference between the mean scores of males and females in the study. The mean scores for males were 26.30, while the mean scores for females 26.92. However, the mean scores for attitude towards healthy sexual practice are significant because we yielded a score of 69.39 for males and females. The attitude scale for females is higher at 3.53 is significant because the One-Way F test is 69.39, which is a very large Score. HIV knowledge does not impact students taking or not taking risk behavior involving sex.
As displayed in Table 5, HIV knowledge does not impact students taking or not taking risk behavior involving sex. There was no correlation between HIV knowledge and risk behavior practices in the sexual relationship. Conversely, safe sex attitude has no impact because the better the attitude the lower the probability of sexual risk in the population of the sample. Besides, safe sex attitudes had a higher correlation of 0.773 between HIV preventive measures and safe sex attitudes. The researchers strongly believe that if the respondents have a good attitude towards safe sex practices, then they would apply preventive HIV sexual measures.
Conclusion
The findings from this investigation should assist HBCUs in developing educational programs and culturally sensitive intervention and prevention strategies aimed at students that are at risk for participating in risky sexual behaviors. The infusion of HIV/AIDS throughout curricula should be mandatory for accredited universities and colleges to avert students and others from acquiring HIV/AIDS. They indicate attitudinal and modeling approaches are more effective than the merely informational usually known as “Sex Education”. This study also contributes more knowledge to the already existing literature surrounding the disproportionately higher incidences of HIV/AIDS among African Americans.
Others findings from this study will contribute to closing the gap related to why African Americans, namely young adults, continue to be affected and infected with HIV. The findings from this study should increase understanding and raise awareness and interest in HIV/AIDS among students and the larger community. Finally, a recommendation to universities administrators and presidents is to be receptive and open to discussing risk-taking behaviors in the form of sexual practices that are impacting students and implementing counseling and risk-reduction programs aimed at all students who attends HBCUs.
Conflicts of Interest (COI) Statement
The author has declared no conflict of interest.
References
Perera UAP, & Abeysena C. (2018). Prevalence and associated factors of risky sexual behaviors among undergraduate students in state universities of Western Province in Sri Lanka: a descriptive cross sectional study. Reproductive Health. 2018 ;( 1). doi: 10.1186/s12978-018-0546-z.View
Yi S, Te V, Pengpid S, & Peltzer K. (2018). Social and behavioural factors associated with risky sexual behaviors among university students in nine ASEAN countries: A multicountry cross-sectional study. Journal of Social Aspects of HIV / AIDS, 15(1). doi:10.1080/17290376.2018.1503967.View
Chanakira E, O’Cathain A, Goyder EC, & Freeman JV. (2014). Factors perceived to influence risky sexual behaviors among university students in the United Kingdom: a qualitative telephone interview study. BMC Public Health. 2014; 14:1-7. doi: 10.1186/1471-2458-14-1055.View
Haile Z, Kingori C, Darlington K-A, Basta T, & Chavan B. (2017). HIV Risk Perception among College Students at a University in the Midwest. Sexuality & Culture, 21(1):62-73. doi: 10.1007/s12119-016-9380-z.View
James TG, & Ryan SJ. (2018). HIV Knowledge Mediates the Relationship between HIV Testing History and Stigma in College Students. Journal of American College Health, 66(7):561-569.View
Pittman DM, Kaur P, & Eyler LT. (2019).Hidden in plain sight: Making a case for heterosexual Black college women being identified as a high-risk population for HIV infection. Cultural Diversity and Ethnic Minority Psychology, 25(1):104-112. doi: 10.1037/cdp0000225.View
Burnett AJ, Sabato TM, Wagner L, & Smith A. (2014). The Influence of Attributional Style on Substance Use and Risky Sexual Behavior among College Students. College Student Journal. 2014; 48(2):325-336.View
Centers for Disease Control and Prevention. HIV Surveillance Report, 2017; vol. 29.View
Murray, A., Haung, M. J., Hardnett, F., & Sutton, M. Y. (2014). HIV knowledge and awareness among undergraduate students at Historically Black College and Universities. Journal of Health Disparities Research and Practice, 7(4), 33-45
Lyttle D, Montgomery AJ, Davis BL, Burns D, McGee ZT, & Fogel J. (2018). An Exploration Using the Neuman Systems Model of Risky Sexual Behaviors among African American College Students: A Brief Report. Journal of Cultural Diversity, 25(4):142-147.View
Murray, A., Huang, M. J., Hardnett, F., & Sutton, M. Y. (2014). Strengthening HIV knowledge and awareness among undergraduate students at Historically Black Colleges and Universities. Journal of Health Disparities Research and Practice, 7(4), 33-45.
Haynes, C. R. (2016). The social cognitive determinants of HIV/AIDS prevention behaviors among baby boomers. Educational Gerontology, 42, 474-482. doi: 10. 1080/03601277.2016.1156385View
Marsiglia FF, Jacobs BL, Nieri T, Smith SJ, Salamone D,& Booth J.(2013). Effects of an Undergraduate HIV/AIDS Course on Students’ HIV Risk. Journal of HIV/AIDS & Social Services, 12(2):172-189. doi:10.1080/15381501.2013.790750.View
Mavhandu-Mudzusi AH, & Asgedom T. (2016). The prevalence of risky sexual behaviors amongst undergraduate students in Jigjiga University, Ethiopia. Health SA Gesondheid, 21:179- 186. doi: 10.1016/j.hsag.2015.11.002.View
Centers for Disease Control (2015). HIV Surveillance Report, 26. Atlanta, GA.
Buckley, TR, & Awais YJ. (2019). Understanding HIV Prevention with College-Going Black Women: An NIMHFunded Pilot Study. Journal of Multicultural Counseling and Development, 47(2):74-89.View
Tung W-C, Cook DM, Lu M, & Ding K. (2015). A Comparison of HIV Knowledge, Attitudes, and Sources of STI Information between Female and Male College Students in Taiwan. Health Care for Women International, 36(8):870-882. doi:10.1080/073 99332.2014.962136.View
Sabato T. (2015). HIV in Young Adults: An Exploration of Knowledge and Risk. College Student Journal. 49(3):427-437
Wang, S. C., Lui, J. H. L., Vega, G., Waldrop, M., & Garris, J. (2018). The Moderating Effect of Alcohol Use on Protective and Risky Sex Behaviors among College Students in the Southeast United States. Journal of American College Health, 66(7), 546–552 View
Carlson GC, & Duckworth MP. (2019). Sexual victimization and benefits expectations of risky behavior among female college students. Journal of Interpersonal Violence, 34 (8):1543-1562. doi: 10.1177/0886260516651626
Burns, D.D. (Producer). (2016, October 28). E=Empathy – Does It Really Make a Difference? [Audio podcast].View"target="blank">View
Burns S. (2015). Sexual health, alcohol and the university environment: is there a need for sexual health promotion intervention? Sexual Health, 12(3):269-271. doi: 10.1071/ SH14215.View
Shiferaw Y, Alemu A, Assefa A, Tesfaye B, Gibermedhin E, & Amare M. (2014). Perception of risk of HIV and sexual risk behaviors among University students: implication for planning interventions. BMC Research Notes ;( 1). doi: 10.1186/1756- 0500-7-162.View
Carey, M. P., Morrison-Beedy, D., & Johnson, B. T. (1997). The HIV-Knowledge Questionnaire: Development and evaluation of a reliable, valid, and practical self-administered questionnaire. AIDS and Behavior, 1, 61-74.View